| Kidney Res Clin Pract > Epub ahead of print |
Abstract
Background
Methods
Results
Supplementary Materials
Notes
Funding
This work was supported in part by a Cooperative Research Grant 2019 from the Korean Society of Nephrology and the Ulsan University Hospital Research Grant (UUH-2020-08). This research was also supported by a grant from the Patient-Centered Clinical Research Coordinating Center (PACEN) funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HC21C0059).
Data sharing statement
The datasets used and/or analyzed during the current study are available upon reasonable request from the corresponding author.
Authors’ contributions
Conceptualization, Methodology, Supervision: SRK, KDY
Data curation: BMY, SK, SRK, KDY
Formal analysis: BMY, SRK
Funding acquisition: YAH, KDY, SHK
Investigation, Resources: WYP, JHC, BCY, MH, SHS, GJK, JWY, SC, YAH, YYH, EB, IOS, HK, WMH, SJS, SHK
Writing–original draft: BMY, SK, SRK, KDY
Writing–review & editing: All the authors
All the authors approved the final version of the manuscript.
Acknowledgments
Figure 1.
Study flow chart.

Figure 2.
Kaplan-Meier survival curve.
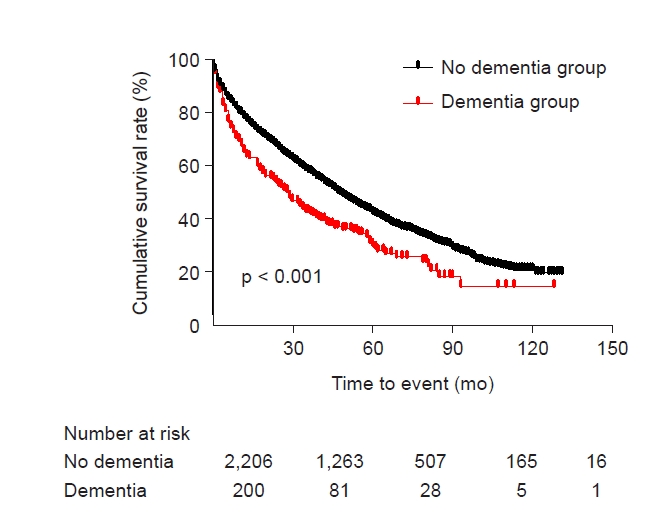
Figure 3.
Subgroup analysis.
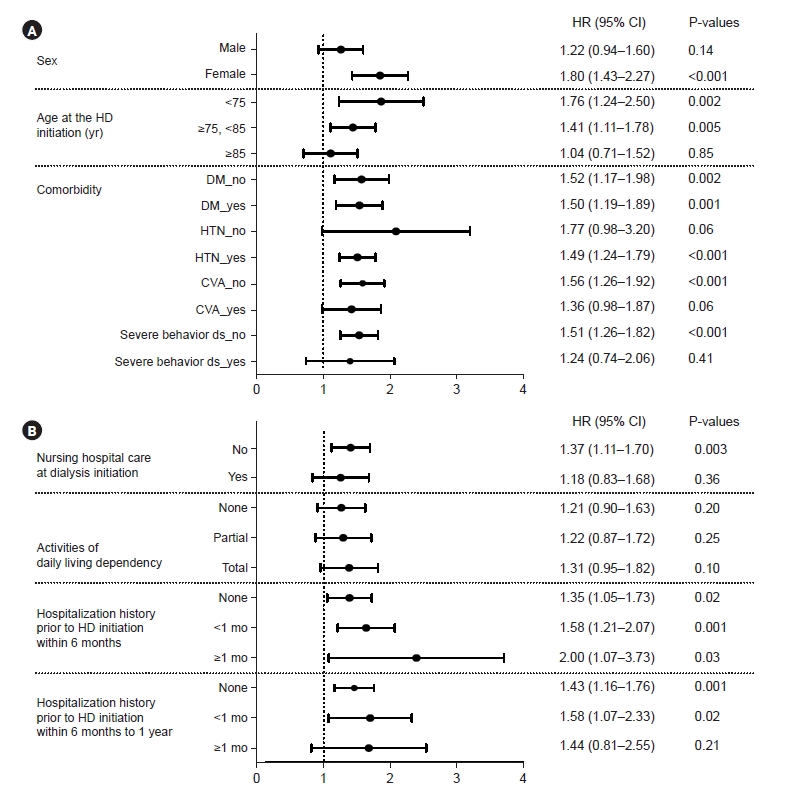
Figure 4.
Survival analysis in the propensity-matched cohort.
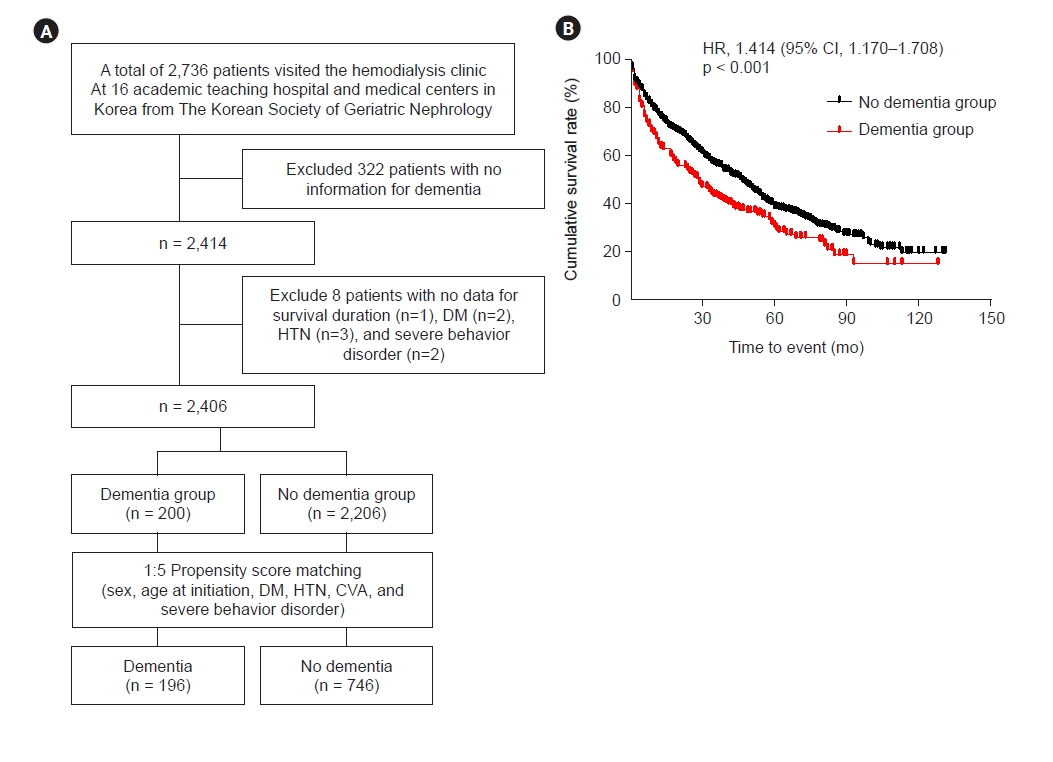
Table 1.
| Charateristic | No dementia group | Dementia group | p-valuea |
|---|---|---|---|
| No. of patients | 2,206 | 200 | |
| Male sex | 1,237 (56.1) | 89 (44.5) | 0.002 |
| Age at hemodialysis initiation (yr) | 77.7 ± 5.5 | 79.6 ± 6.0 | <0.001 |
| Primary etiology | |||
| Diabetes mellitus | 1,052 (47.7) | 91 (45.5) | 0.25 |
| Glomerulonephritis | 195 (8.8) | 10 (5.0) | |
| Renovascular disease | 561 (25.5) | 59 (29.5) | |
| Others | 398 (18.0) | 40 (20.0) | |
| Vascular access at dialysis initiation | |||
| Temporary catheter | 1,777 (80.6) | 179 (89.5) | <0.001 |
| AVF | 342 (15.5) | 11 (5.5) | |
| AVG | 80 (3.6) | 10 (5.0) | |
| Others | 7 (0.3) | 0 (0) | |
| Vascular access on maintenance initiation | |||
| Temporary catheter | 390 (17.7) | 73 (36.5) | <0.001 |
| AVF | 1,436 (65.1) | 78 (39.0) | |
| AVG | 355 (16.1) | 43 (21.5) | |
| Others | 25 (1.1) | 6 (3.0) | |
| Malignancy | |||
| None | 1,850 (83.9) | 173 (86.5) | 0.33 |
| Curative state | 302 (13.7) | 20 (10.0) | |
| Ongoing treatment | 30 (1.4) | 4 (2.0) | |
| Palliative treatment | 24 (1.1) | 3 (1.5) | |
| Lymphoma | 22 (1.0) | 0 (0) | 0.25 |
| Ischemic heart disease | 487 (22.1) | 38 (19.0) | 0.47 |
| Peripheral artery disease | 158 (7.2) | 8 (4.0) | 0.12 |
| Cerebrovascular accident | 436 (19.8) | 68 (34.0) | <0.001 |
| Congestive heart failure | 427 (19.4) | 36 (18.0) | 0.70 |
| Atrial fibrillation | 213 (9.7) | 25 (12.5) | 0.24 |
| Diabetes mellitus | 1,282 (58.1) | 111 (55.5) | 0.52 |
| Hypertension | 1,951 (88.4) | 185 (92.5) | 0.10 |
| Severe behavioral disorder | 112 (5.1) | 32 (16.0) | <0.001 |
| Hospitalization history prior to dialysis initiation within 6 months | |||
| None | 1,427 (64.7) | 103 (51.5) | 0.001 |
| <1 mo | 675 (30.6) | 82 (41.0) | |
| ≥1 mo | 103 (4.7) | 15 (7.5) | |
| Hospitalization history from 6 months to 1 year prior to dialysis initiation | |||
| None | 1,850 (83.9) | 139 (69.5) | <0.001 |
| <1 mo | 293 (13.3) | 42 (21.0) | |
| ≥1 mo | 62 (2.8) | 19 (9.5) | |
| Nursing facility care at dialysis initiation | |||
| No | 1,875 (91.5) | 140 (72.9) | <0.001 |
| Yes | 174 (8.5) | 52 (27.1) | |
| Laboratory findings | |||
| WBCs (/mm3) | 9,291.9 ± 17,514.7 | 9,396.3 ± 4,282.1 | 0.83b |
| Hemoglobin (g/dL) | 9.2 ± 2.2 | 9.2 ± 1.7 | 0.81b |
| Glucose (mg/dL) | 151.2 ± 74.1 | 154.0 ± 80.3 | 0.62b |
| BUN (mg/dL) | 80.4 ± 34.2 | 79.0 ± 39.6 | 0.62b |
| Creatinine (mg/dL) | 6.5 ± 2.9 | 5.9 ± 2.7 | 0.004b |
| Albumin (g/dL) | 3.4 (3.0–3.8) | 3.2 (2.8–3.6) | <0.001c |
| Total bilirubin (mg/dL) | 0.5 ± 0.9 | 0.5 ± 1.3 | 0.77b |
| Total cholesterol (mg/dL) | 144.7 ± 47.8 | 141.0 ± 44.6 | 0.32b |
References
- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 447 View
- 33 Download
- ORCID iDs
-
Byung Min Ye

https://orcid.org/0000-0002-0751-8895Seongmin Kang

https://orcid.org/0000-0001-7566-5339Woo Yeong Park

https://orcid.org/0000-0003-2662-2898Jang-Hee Cho

https://orcid.org/0000-0002-7031-5214Byung Chul Yu

https://orcid.org/0000-0002-2686-1904Miyeun Han

https://orcid.org/0000-0001-7304-2496Sang Heon Song

https://orcid.org/0000-0002-8218-6974Gang-Jee Ko

https://orcid.org/0000-0001-8355-1083Jae Won Yang

https://orcid.org/0000-0003-3689-5865Sungjin Chung

https://orcid.org/0000-0002-9886-8339Yu Ah Hong

https://orcid.org/0000-0001-7856-4955Young Youl Hyun

https://orcid.org/0000-0002-4204-9908Eunjin Bae

https://orcid.org/0000-0001-6890-4725In O Sun

https://orcid.org/0000-0001-7245-3736Hyunsuk Kim

https://orcid.org/0000-0003-1889-253XWon Min Hwang

https://orcid.org/0000-0001-7548-6111Sung Joon Shin

https://orcid.org/0000-0002-0777-9278Soon Hyo Kwon

https://orcid.org/0000-0002-4114-4196Seo Rin Kim

https://orcid.org/0000-0003-3552-0519Kyung Don Yoo

https://orcid.org/0000-0001-6545-6517 - Related articles
-
Association between hearing loss and physical performance in patients on maintenance hemodialysis
The impact of severe depression on the survival of older patients with end-stage kidney disease



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Supplement table 1
Supplement table 1 Print
Print















