Korean Society of Nephrology 2022 Recommendations on controversial issues in diagnosis and management of hyponatremia
Article information
Abstract
The Korean Society for Electrolyte and Blood Pressure Research, in collaboration with the Korean Society of Nephrology, has published a clinical practice guideline (CPG) document for hyponatremia treatment. The document is based on an extensive evidence-based review of the diagnosis, evaluation, and treatment of hyponatremia with the multidisciplinary participation of representative experts in hyponatremia with methodologist support for guideline development. This CPG consists of 12 recommendations (two for diagnosis, eight for treatment, and two for special situations) based on eight detailed topics and nine key questions. Each recommendation begins with statements graded by the strength of the recommendations and the quality of the evidence. Each statement is followed by rationale supporting the recommendations. The committee issued conditional recommendations in favor of rapid intermittent bolus administration of hypertonic saline in severe hyponatremia, the use of vasopressin receptor antagonists in heart failure with hypervolemic hyponatremia, and syndrome of inappropriate antidiuresis with moderate to severe hyponatremia, the individualization of desmopressin use, and strong recommendation on the administration of isotonic fluids as maintenance fluid therapy in hospitalized pediatric patients. We hope that this CPG will provide useful recommendations in practice, with the aim of providing clinical support for shared decision-making to improve patient outcomes.
Introduction
Hyponatremia, defined as serum sodium (SNa) concentration of <135 mmol/L, is the most frequent body fluid and electrolyte balance disturbance encountered in clinical practice. Although several international guidelines for managing hyponatremia are available, the differential diagnosis of hyponatremia is frequently challenging in patients with complex clinical settings and varying treatment. To assist patients, clinicians, and other healthcare professionals with decisions about the diagnostic approach to and treatment of hyponatremia, a multidisciplinary guideline development committee representing specialists with a genuine interest in hyponatremia was convened by the Korean Society for Electrolyte and Blood Pressure Research in collaboration with the Korean Society of Nephrology clinical practice guideline (CPG) committee. The development committee has developed the CPG and applied strict management strategies to minimize potential bias. The committee prioritized clinical questions and outcomes according to their importance for clinicians and patients. The committee used the Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach, including GRADE Evidence-to-Decision frameworks, to assess evidence and make recommendations. The level of evidence for each result is graded as high/moderate/low/very low. The recommendation grade was divided into four levels: strong recommendation (A), conditional recommendation (B), against recommendation (C), and inconclusive (I). Definitions of the evidence levels are shown in Table 1. The key questions that cannot be adapted or developed directly due to the limitations of existing research are expressed as expert consensus (E). In addition to a rigorous approach to methodology and evaluation, this document represents recommended approaches for multiple etiologies of hyponatremia based on both the consensus opinions of experts in hyponatremia and the most recent published data in this field. There is also a link to full-text documents and lists of the most important reports so that the readers can obtain further information (most of which is available online).
Recommendations on diagnostic procedures
Classification of hyponatremia
Hyponatremia is defined by less than 135 mmol/L of SNa [1]. Hyponatremia can be classified based on different parameters, including SNa concentration, timing of development, symptom severity, serum osmolality, and volume status. The criteria are described in Table 2 [1–3]. Because consistency and clarity of classification of hyponatremia are critical for diagnosis and management, we sought to compare the terminology used in the existing two guidelines (European and American guidelines) when discussing the classification of hyponatremia (Table 2).
Differential diagnosis of hyponatremia
A practical diagnostic approach can progress step by step as follows (Fig. 1) [1].
1) Step 1
Check plasma osmolality for differentiating hypoosmolar hyponatremia from other causes of hyponatremia [1,3]. When plasma osmolality is reduced, you may require further steps of differential diagnosis. When plasma osmolality is above 275 mOsm/kg and hyponatremia is present, hyperglycemia should be checked. When serum glucose levels are increased, recheck the corrected sodium level according to the correction formula.
Corrected Na level (Hillier et al. [4]) = Na + 0.024 × (serum glucose [mg/dL] – 100)
Beyond hyperglycemia, hyperproteinemia, hyperlipidemia, and the use of mannitol or radiocontrast media can be a cause of hyper- or iso-osmolar hyponatremia [1–3].
2) Step 2
When hypoosmolar hyponatremia has been confirmed, the severity of clinical hyponatremic symptoms should be evaluated [1]. We have divided symptoms of hyponatremia into ‘asymptomatic-mild,’ ‘moderate,’ and ‘severe’ categories (Table 2). Symptomatic hyponatremia should be corrected immediately with acute management [1]. If acute management has been initiated or there are no symptoms of hyponatremia, go to the next step.
3) Step 3
Check urinary osmolality and discriminate excessive water intake.
When urinary osmolality is below 100 mOsm/kg, discriminate excessive water intake and excessive intake of hypotonic food or fluid (e.g., beer, rice wine, liquid diet) [1–3].
4) Step 4
Check urinary sodium to discriminate excessive renal excretion of sodium. When urinary sodium is above 30 mmol/L, discriminate the cause of hyponatremia according to volume status [1,3]. When volume status is decreased, check use of diuretics and cerebral salt wasting (CSW). When volume status is normal, check adrenal insufficiency, hypothyroidism, syndrome of inappropriate antidiuresis (SIAD), and other diseases or drugs that can cause SIAD.
When urinary sodium is below 30 mmol/L, recheck volume status and discriminate the causes. When volume status is decreased, check diarrhea or vomiting. When volume status is increased, discriminate congestive heart failure, liver cirrhosis, and nephrotic syndrome.
Volume status can be assessed through history-taking and physical examination. Symptoms of decreased volume status are usually nonspecific and may include thirst, fatigue, weakness, muscle cramps, and orthostatic dizziness. On physical examination, decreased skin turgor, low jugular vein pressure, orthostatic hypotension or postural tachycardia may appear. When more body fluid is lost, findings suggestive of decreased organ perfusion due to decreased intravascular fluid (low consciousness, oliguria, and peripheral cyanosis) or compensatory mechanisms (tachycardia, tachypnea, and sweating) may appear as symptoms of shock. On laboratory findings, increased urine osmolality, decreased urine sodium (UNa), alkalosis due to decreased volume status, relatively increased hemoglobin and albumin concentration may also be seen. Symptoms of increased volume status may include dyspnea on exercise, orthopnea, and peripheral edema. After underlying causes are evaluated, take further steps for managing them [1,3].
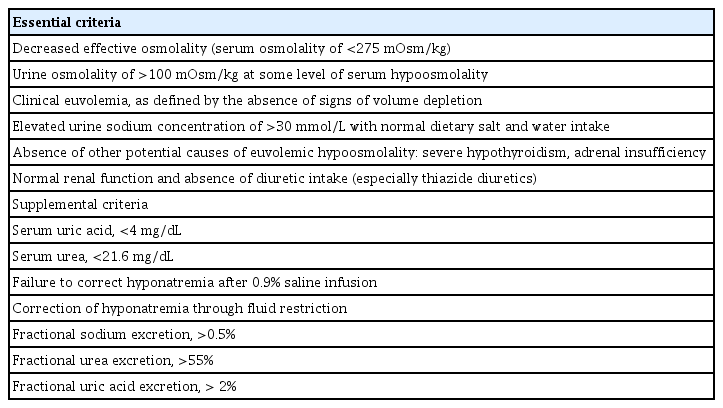
The diagnostic criteria of SIAD are summarized in Table 3 [1,2]. In addition, fractional excretion of uric acid (FEUA) can be used for discrimination of SIAD and use of diuretics (Recommendation 1) [3]. Serum copeptin/UNa ratio may also be used for discrimination of volume status. However, practical applications are still limited since copeptin measurement is not widely used (Recommendation 2).
Diagnostic approaches should be performed step by step, including measuring plasma osmolality, urinary osmolality, and urinary sodium levels. Patient history and physical examination are also important to discriminate underlying causes of hyponatremia. Drug history should also be checked, as it can be associated with hyponatremia including SIAD [1].
For example, thiazide diuretics are a common cause in elderly women, and desmopressin in elderly men [5,6]. In patients with chronic pain, NSAID use should be checked. In patients with skin disorders or autoimmune diseases, adrenal insufficiency should be evaluated.
Recommendation 1
For patients with hyponatremia, we consider additional measurement of FEUA reasonable to differentiate likely causes of hyponatremia, such as SIAD or diuretic-induced hyponatremia (E).
Remarks:
1. FEUA was significantly higher in SIAD patients than in patients taking diuretics.
2. When patients taking diuretics were divided into thiazide and loop diuretics, SIAD- and thiazide-induced hyponatremia showed similar FEUA values.
FEUA is a supplemental diagnostic criterion for SIAD [7]; in patients using diuretics, FEUA performed best among UNa, fractional excretion of sodium (FENa), fractional urea excretion, and serum uric acid concentration (area under the curve, 0.96; 0.92–1.12) [8]. In the 2013 guideline published by the American Journal of Medicine, the measurement of FEUA in patients taking diuretics has been suggested to be helpful when trying to exclude hypovolemia [2]. According to the 2014 European guideline from the European Society of Endocrinology, European Society of Intensive Care Medicine, and European Renal Association European Dialysis and Transplant Association, FEUA using a threshold of >12% was most useful for distinguishing SIAD- from non-SIAD-related hyponatremia in patients on diuretics with a sensitivity of 0.86 and specificity of 1.00 [1]. However, the previous guidelines had no evidence derived from high-quality randomized controlled trials (RCTs). Our literature search identified two new observational studies from 2014 when the previous guideline was published.
In an observational study of 298 patients admitted with profound hypoosmolar hyponatremia (Na of <125 mmol/L), FEUA was higher in patients with SIAD compared with other hyponatremia etiologies (p < 0.001) [9]. We identified direct evidence from five observational studies (387 patients) that interpreted FEUA and FENa in hyponatremia patients due to SIAD and on diuretics [8-12]. Of these, one study was conducted with only patients taking thiazide diuretics, and in the other four studies, the group of patients taking thiazide or loop diuretics was not separated in our meta-analysis. A meta-analysis of studies showed that FEUA was significantly higher in SIAD patients than in patients taking diuretics. Two of five observational studies identified FEUA cutoff values of 10% and 12% (with specificity of 100% and 96%, respectively) [9,10]. Our meta-analysis found no differences in FENa. Since uric acid transporters are mostly located in the proximal tubules of the kidney, in which diuretics do not work primarily, we consider it reasonable that FEUA be used as a diagnostic test for the differential diagnosis of hyponatremia. However, caution is needed in interpreting FEUA. When patients taking diuretics were divided into thiazide and loop diuretics, SIAD- and thiazide-induced hyponatremia showed similar FEUA values in one study [10]. Furthermore, hypouricemia with increased FEUA is also observed in CSW. FEUA can be normalized after correction of hyponatremia in SIAD despite the continued increase in FEUA in CSW [13]. Lastly, concurrent use of drugs such as antihypertensives that alter uric acid excretion may affect FEUA levels [14]. Further evidence is needed to address the role of FEUA in diuretic-induced hyponatremia.
Recommendation 2
There are insufficient data to make a recommendation for using copeptin to UNa ratio to assess patient volume status (I, very low).
Remarks:
1. Copeptin levels overlap widely in hyponatremic patients and are affected by non-osmotic stimuli.
2. The ratio of copeptin to UNa was higher in disorders with secondary arginine vasopressin (AVP) release than those with primary AVP secretion such as SIAD.
Assessment of volume status in hyponatremic patients is important, but often challenging. Since the sensitivity and specificity of traditional clinical assessment of patient volume status are low, there have been efforts to identify novel biomarkers. Plasma AVP is a promising marker for the differentiation of volume disorders from a pathophysiological perspective. However, AVP is not routinely measured in clinical practice due to its instability. Copeptin has become a surrogate maker for AVP concentration and has advantages over AVP in aspects of stability and ease of measurement. Both American and European guidelines discussed copeptin briefly [1,2]. The American (2013) and European (2014) guidelines recommend that measurement of the copeptin to UNa ratio could distinguish hypovolemic hyponatremia from SIAD and that copeptin could discriminate euvolemia from hypovolemia and hypervolemia. Both guidelines were developed based on the same observational study [15]. There were no RCTs or meta-analyses exploring the value of copeptin in patients with hyponatremia. In the present guideline, one observational study published after 2015 was added and discussed [16].
Since copeptin levels overlap widely in hyponatremic patients and are affected by nonosmotic stimuli, copeptin to UNa ratio can be useful. In a previous report of 106 German hyponatremia patients, patients were classified into five categories: 1) normal volume with excessive water intake; 2) normal volume with SIAD; 3) decreased volume due to renal sodium loss; 4) decreased or normal volume due to non-renal sodium loss; and 5) increased volume [15]. A recent study of 100 Korean hyponatremic patients also classified patients into five categories: 1) normal volume with adrenal insufficiency; 2) normal volume with SIAD; 3) decreased volume due to renal sodium loss; 4) decreased volume due to non-renal sodium loss; and 5) increased volume [16]. Both observational studies revealed that copeptin to UNa ratio was superior to copeptin level for differentiating patient volume status. The ratio of copeptin to UNa was higher in disorders with secondary AVP release (decreased effective arterial volume) than conditions with primary AVP secretion such as SIAD.
Recommendations on treatment issues
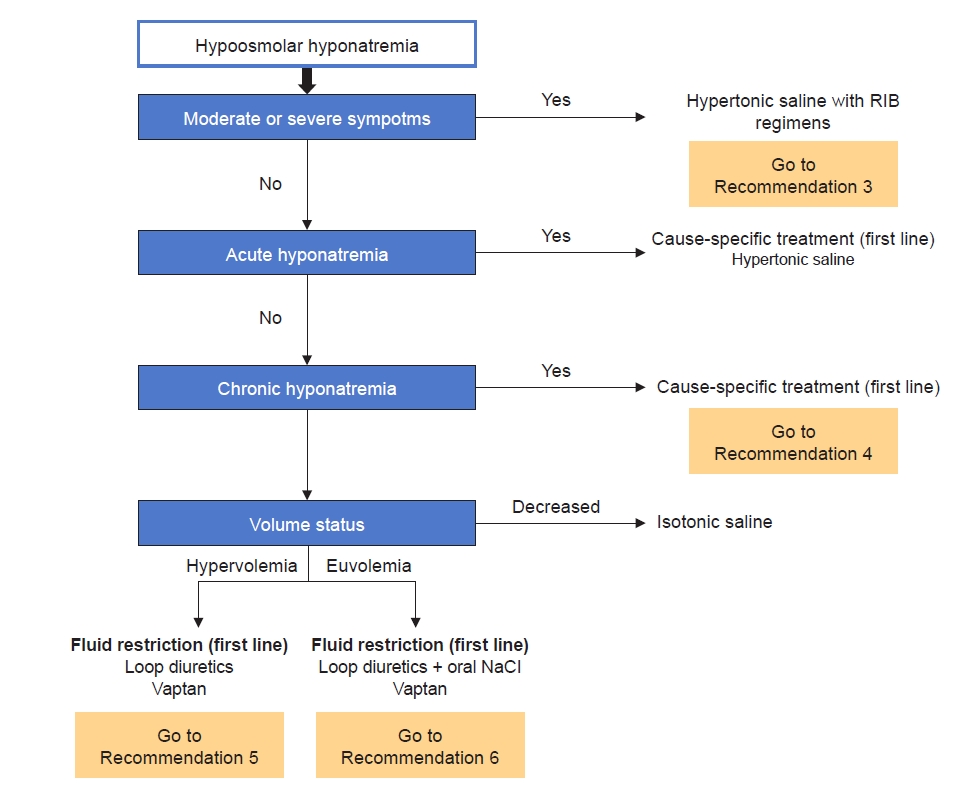
The first step treatment evaluation of hyponatremia is identifying clinical symptoms and duration of hyponatremia, as mentioned above [1]. Treatment can be approached step by step as follows (Fig. 2).
1) Symptomatic acute/chronic hyponatremia
Hypertonic saline should be administered for symptomatic hyponatremia as moderate or severe symptomatic hyponatremia reflects increased intracranial pressure. In terms of the infusion method of hypertonic saline, rapid intermittent bolus (RIB) regimens are suggested [1,2]. The treatment approach used for hypertonic saline in the American and European guidelines, and in a recent RCT performed in Korea is as follows (Table 4) [1–3,17]. A comparison of the efficacy and safety of hypertonic saline according to infusion methods (RIB vs. slow continuous infusion [SCI]) is discussed in Recommendation 3.
Recommendation 3
We suggest RIB administration of hypertonic saline in patients with symptomatic severe hypotonic hyponatremia (B, low).
Remarks:
In the treatment of symptomatic severe hypotonic hyponatremia,
1. RIB administration of hypertonic saline can effectively relieve symptoms within 12 hours compared to SCI.
2. RIB is more effective in increasing SNa within 1 hour and reaching the target correction rate than SCI.
3. RIB can result in a lower incidence of therapeutic re-lowering of SNa than SCI.
4. RIB has similar overcorrection, osmotic demyelination syndrome (ODS), and mortality rates to SCI.
Hypertonic saline has been used to treat symptomatic severe hypotonic hyponatremia. Overcorrection from indiscriminate prolonged use of hypertonic saline may result in irreversible neurologic sequelae from ODS, whereas under-correction of hyponatremia may insufficiently improve fatal complications of cerebral edema. Therefore, appropriate correction of SNa is needed. Although the American (2013) and European (2014) guidelines recommend administering hypertonic saline in small, fixed boluses (recommendation grade: expert opinion in the American guidelines, 1D in the European guidelines), they were not based on high-quality RCT evidence [1,2,17]. In order to examine whether RIB therapy of hypertonic saline has any benefit for symptom relief, correction of SNa, complications, and prognosis compared to SCI in patients with symptomatic severe hypotonic hyponatremia, we reviewed a prospective cohort study (24 hours of follow-up after treatment) and a RCT (48 hours of follow-up after treatment) published after the European guideline (2014).
A prospective cohort study reported that the RIB group had more rapid elevation of SNa and greater improvement in the Glasgow Coma Scale (GCS) at 6/12 hours than the SCI group. However, there was no difference between the two groups in GCS improvement at 24 hours [18].
A RCT demonstrated that the RIB group had the higher increment in SNa at 1 hour, a higher proportion meeting the target correction rate (achieving SNa of 5–9 mmol/L within 24 hours and SNa of 10–17 mmol/L or ≥130 mmol/L within 48 hours) at 1 hour, lower SNa at 12 hours, and a lower incidence of re-lowering treatment (5% dextrose infusion 10 mL/kg over 1 hour and/or intravenous desmopressin 2 µg if SNa level increase is ≥10 mmol/L within the first 24 hours or ≥18 mmol/L within 48 hours) than the SCI group [17].
In both studies, the target correction rate, the degree of SNa elevation at 24 hours, and overcorrection (increase in SNa by >12 mmol/L within the first 24 hours or increase in SNa by >18 mmol/L within 48 hours) did not differ between the two groups [17,18]. ODS did not occur in either study [17,18]. Death occurred in five patients in the RCT and four patients in the prospective cohort study, with no significant difference between the two groups [17,18]. Only one RCT for hypertonic saline infusion in symptomatic severe hypotonic hyponatremia has been reported in Korea; thus, additional large-scale RCTs are needed.
In cases of severe symptomatic hyponatremia, RIB regimens of hypertonic saline should be promptly administered to increase SNa by 4 to 6 mmol/L to relieve cerebral edema, and then cause-specific treatment can be planned [1]. In cases of moderate symptomatic hyponatremia, RIB or SCI methods of hypertonic saline can be used and cause-specific treatment can be prioritized without administration of hypertonic saline [1]. We suggest checking SNa concentration 1 hour after first hypertonic saline administration, then rechecking SNa concentration every 6 hours to adjust the administration interval or infusion rate of hypertonic saline [1]. We recommend that the rate of sodium correction be reevaluated when symptoms improve or SNa concentration increases by 5 to 9 mmol/L [1,2]. If symptoms do not improve or SNa concentrations do not reach target correction, infusion of hypertonic saline may be repeated [1,2]. In patients with hypervolemic hyponatremia, hypertonic saline and loop diuretics should be administered at the same time [3].
2) Asymptomatic acute hyponatremia
The absence of moderate or severe symptoms indicates that the clinically significant brain edema has not yet developed. Therefore, prompt diagnostic assessment of hyponatremia is suggested versus immediate infusion of hypertonic saline. Nonessential fluids and medications that can contribute to or provoke hyponatremia should be stopped. If the acute decrease in SNa concentration exceeds 10 mmol/L, we suggest administering the same amount of hypertonic saline as in patients with moderate symptoms to prevent a further drop in SNa concentration [1].
3) Asymptomatic chronic hyponatremia
Asymptomatic chronic hyponatremia does not require prompt correction but may lead to localized neurologic impairment and increased mortality compared to normonatremia. Even patients with mild hyponatremia have a higher mortality rate compared to patients with normonatremia.
Recommendation 4
We recommend rigorously evaluating the causes of mild hyponatremia and to managing causative diseases to improve clinical outcomes (E).
Remarks:
1. Mild hyponatremia increases the risk of mortality compared with those with normonatremia.
2. There is no clear evidence that correcting hyponatremia itself improves patient-important outcomes.
3. There are insufficient data to make a recommendation regarding treating mild hyponatremia with hypertonic saline or oral sodium chloride solely to increase SNa concentration.
In the case of mild hyponatremia, it is often unnoticed in clinical practice because it rarely presents with specific symptoms. Moreover, there is lack of evidence from RCTs that treatment of mild hyponatremia with fluid therapy or medication with the sole aim of correction to normal SNa concentration improves patient outcomes. The European guideline (2014) recommends against treatment simply to increase SNa concentration (grade of recommendation 2C). However, several observational studies have shown that mild hyponatremia increases the risk of mortality both in short-term and long-term follow-up. Waikar et al. [19] reported that hospitalized patients with mild hyponatremia defined as a SNa concentration of 130 to 134 mEq/L showed increased in-hospital mortality risk compared with those with normonatremia. Doshi et al. [20] found that hospitalized cancer patients with mild hyponatremia showed two-fold increased risk of morality compared to those with normonatremia. Furthermore, Kovesdy et al. [21] observed that mild hyponatremia defined as 130 to 135.9 mEq/L increased the risk of relatively long-term mortality (median follow-up duration, 5.5 years) in patients with chronic kidney disease with estimated glomerular filtration rate less than 60 mL/min/1.73 m2. From a meta-analysis including above studies that compared the short-term (less than 90 days or in-hospital mortality) and long-term (more than 5 years mortality) mortality risk, mild hyponatremia increased both short-term (odds ratio [OR], 2.09; 95% confidence interval [CI], 1.90–2.30; p < 0.001) and long-term (OR, 1.46; 95% CI, 1.44–1.48; p < 0.001) mortality risk compared with normonatremia.
In a domestic retrospective study [22], improved SNa concentration at discharge had the strongest association with long-term mortality in acute myocardial infarction patients with hyponatremia. However, because mild hyponatremia patients were not distinguished from other study patients, and interventions such as hypertonic saline were not addressed in this study, these findings were not included in the rationale under the consensus of the Development Committee. Although there is insufficient data that the correction of mild hyponatremia with the sole aim of correcting SNa concentration has clinical benefit, it is reasonable to rigorously evaluate the causes of mild hyponatremia and to manage the diseases because mild hyponatremia increases the risk of mortality.
(1) Hypervolemic hyponatremia is commonly seen in heart failure or liver cirrhosis. Restriction of sodium and free water intake (approximate <800–1,000 mL/day) is the first-line treatment. Additional pharmacologic therapies including loop diuretics and vasopressin receptor antagonists (‘vaptans’) can be used to increase renal free water excretion [1–3]. The possibility of using vaptans in patients with heart failure or liver cirrhosis is discussed greater detail in Recommendation 5. Fluid intake should not be restricted to prevent overcorrection when using vaptans [2].
Recommendation 5
1. We suggest vaptan use in heart failure with hypervolemic hyponatremia in terms of rapid sodium correction (B, moderate).
2. We make no recommendation on the use of vaptans in liver cirrhosis with hypervolemic hyponatremia (E).
Remarks:
1. We evaluated the efficacy of adding vaptans to loop diuretics since few studies compared vaptans versus loop diuretics in heart failure with hypervolemic hyponatremia.
2. The addition of vaptans to loop diuretics is more effective to elevate SNa concentration compared with loop diuretics alone.
3. The addition of vaptans to loop diuretics does not worsen renal function compared with loop diuretics alone.
4. The addition of vaptans to loop diuretics does not show survival benefit compared with loop diuretics alone.
5. The addition of vaptans has the potential to lead to hepatotoxicity in patients with liver cirrhosis.
Although vaptans have shown effectiveness for correcting SNa in SIAD, heart failure, and liver cirrhosis, the U.S. Food and Drug Administration (FDA) limited the use of vaptans in liver cirrhosis in 2013 due to hepatic toxicity concerns. The European guideline recommended against treating vaptans in hypervolemic hyponatremia (grade of recommendation 1C). Therefore, we accepted the previous guideline in hyponatremia in liver cirrhosis and did not seek further evidence. We reviewed only patients with heart failure, excluding studies on liver cirrhosis patients.
Including 11 RCTs, one observational study, and two systematic reviews (SRs), the guideline found no clinical benefit to the use of vaptans in hypervolemic hyponatremia. However, the quality of the studies varied, the characteristics of enrolled patients were not similar, and most of the RCTs did not distinguish patients with hypervolemia from those with normal volume status. Also, two studies only included patients with liver cirrhosis, and three studies only enrolled patients with heart failure. Thus, it is difficult to conclude that vaptans are superior to loop diuretics. Although vaptans showed a clinical benefit compared with placebo in the two SRs, there was no comparison of vaptans with loop diuretics as a basic therapeutic agent in hypervolemic hyponatremia. Since 2015, various studies have investigated whether additional use of vaptans with loop diuretics could lead to clinical benefit in hyponatremia with heart failure. Only one study compared vaptans and loop diuretics [23], and nearly all studies sought to clarify the effectiveness of additional vaptan use on loop diuretics. Recent studies showed the efficacy of vaptans in patients with chronic kidney disease and heart failure [24,25].
Therefore, this guideline focused on the benefit of additional vaptan use with loop diuretics in hypervolemic hyponatremia with heart failure in terms of survival gain, sodium correction, and conservation of renal function. We reviewed nine RCTs [23–31], five SRs, and several observational studies. All RCTs were conducted in patients with hyponatremic heart failure prescribed tolvaptan 7.5 to 30 mg per day, and allowed furosemide intravenous or oral use. There was no survival benefit of adding tolvaptan on furosemide [23,25,26,29,31]. Renal function decline, which was defined as the increase of serum creatinine more than 0.3 mg/dL per week, was not different between the tolvaptan-added group and furosemide-alone group [23,26,27,30]. Sodium correction for 24 hours was higher when tolvaptan was added to furosemide [25–27].
(2) SIAD is a state of water retention due to a persistent increase in antidiuretic hormone, characterized by hypoosmolar hyponatremia, euvolemia, and high urine osmolarity. In patients with SIAD, the standard treatment is the restriction of free water because of water retention [32]. The following can be considered second-line treatment: a combination of oral sodium chloride (NaCl) and loop diuretics or vaptans (Recommendation 6) [2,3]. NaCl causes an electrolyte diuresis by increasing urine solute load. However, its primary role is the restoration of urinary sodium losses and preventing negative sodium balance in hyponatremia [33]. NaCl is available as 1 g (17 mEq sodium and chloride) tablets. Usual doses for NaCl tablets are 6 to 9 g daily in divided doses (e.g., 2–3 g two or three times per day). Loop diuretics decrease the medullary osmotic gradient necessary for water reabsorption in the collecting duct by inhibiting the Na-K+-2Cl– cotransporter and therefore, increase free water excretion. The dose of furosemide is 20 to 40 mg per oral one time per day. They are not approved by the U.S. FDA to treat hyponatremia. Daily intake of 0.25 to 0.50 g/kg urea or 600 to 1,200 mg demeclocycline can also be considered but has not been introduced in Korea.
Recommendation 6
We suggest treatment with vaptans in SIAD patients with moderate to severe hyponatremia (B, low).
Remarks:
1. There is no direct comparison of vasopressin receptor antagonists with loop diuretics in patients with SIAD. We compared the effects of vasopressin receptor antagonists with water restriction or placebo.
2. Vaptans have a beneficial effect on normalization of SNa in SIAD patients compared with water restriction or placebo.
3. Vaptans do not increase the risk of overcorrection of hyponatremia in SIAD patients compared with water restriction or placebo.
4. Vaptans do not improve survival in SIAD patients compared with water restriction or placebo.
Vaptans correct hyponatremia, effectively causing urinary excretion of free water without increased sodium excretion [34]. However, the European guideline recommends against vasopressin receptor antagonists in SIAD patients without severe or moderately severe symptoms. They emphasized that the safety of vaptans should be considered. First, vaptans can lead to overcorrection of SNa concentration, especially in patients with severe hyponatremia. Second, hepatotoxicity was reported in autosomal dominant polycystic kidney disease patients on high doses of tolvaptan [1].
Previous studies focused on short-term outcomes such as normalization of SNa or overcorrection. Few studies evaluated the effect of vaptans stratified by volume status: hypervolemia or euvolemia [35,36]. Aggravation of hyponatremia can cause severe symptoms such as poor oral intake, general weakness or altered consciousness, leading to hospitalization. Long-term outcomes were worse in patients who developed repeated symptoms of hyponatremia [19,37].
Placebo or water restriction was used as a control group for vaptans, as there were no studies comparing vaptans with loop diuretics in the previous guidelines or our literature search. Therefore, we reviewed 12 RCTs evaluating the effect of vaptans on sodium correction, survival or complications compared with water restriction or placebo [3,38–48]. All RCTs included euvolemic hyponatremia patients: three included only euvolemic hyponatremia, nine included euvolemic or hypervolemic patients. In our meta-analysis, vaptans effectively normalized SNa in euvolemic hyponatremia. Vaptans did not decrease mortality in euvolemic hyponatremia. Although data on complications of vaptans are insufficient, vaptans did not increase the risk of overcorrection of hyponatremia compared with water restriction or placebo. There were few data regarding hepatotoxicity in euvolemic hyponatremia. In conclusion, vaptans can effectively normalize SNa concentration without increased risk of overcorrection or death.
The evidence was low quality and grade (B) in this recommendation because the included participants were not clearly defined as having SIAD, but instead as hypoosmolar hyponatremia with euvolemia or hypervolemia in the included RCTs. However, most euvolemic hyponatremia is SIAD and the diagnostic criteria for SIAD are not clearly defined [49]. Experts agreed that most of included participants might have SIAD. Therefore, we suggest using vaptans in SIAD patients with moderate to severe hyponatremia.
(3) In patients with hypovolemic hyponatremia, restoring extracellular fluid volume with intravenous isotonic fluid (0.9% saline) or balanced crystalloid will suppress vasopressin secretion causing electrolyte-free water excretion to increase [1–3]. After a 0.5 to 1.0 L infusion of isotonic fluid or balanced crystalloid, hyponatremia will begin to be corrected without signs of volume overload in patients with hypovolemic hyponatremia [2].
4) Overcorrection and re-lowering treatment of serum sodium
Target correction is achieving a SNa increase of 5 to 9 mmol/L/10 to 17 mmol/L within the first 24/48 hours or reaching a SNa of 130 mmol/L [1]. SNa concentration should not be corrected by ≥10 mmol/L per day, with a more stringent limit of >8 mmol/L per day for patients at high risk of ODS (SNa concentration of ≤105 mmol/L, hypokalemia, alcoholism, malnutrition, and advanced liver disease) [2]. Overcorrection (defined as an increase in the SNa level by >12/18 mmol/L within 24/48 hours) may result in ODS [1–3]. ODS has no specific treatment and has a poor prognosis. Therefore, caution is required when correcting hyponatremia [1]. We recommend discontinuing ongoing treatment and prompt intervention to re-lower SNa concentration based on electrolyte-free water (5% dextrose solutions) and/or desmopressin if overcorrection occurs (Table 4) [1–3]. Desmopressin use as a re-lowering treatment for SNa is discussed in Recommendation 7. Diuresis as a result of antagonizing vasopressin-mediated free water retention by volume repletion or discontinuing hyponatremia inducing medications often occurs when correcting hyponatremia and is a common reason for overcorrection. Therefore, urine output should be monitored during treatment.
Recommendation 7
We suggest that desmopressin should be applied individually according to risk factors affecting overcorrection, hypertonic saline therapeutic regimen, and whether to administer dextrose solution during overcorrection in patients with hyponatremia (B, very low).
RRemarks:
1. There is no evidence that administration of desmopressin as a proactive or reactive strategy is effective for preventing overcorrection.
2. Administration of desmopressin in patients with hyponatremia has the potential to increase the incidence of ODS compared to no administration, but drawing a valid conclusion is difficult due to the low level of evidence.
3. Administration of desmopressin for the prevention of overcorrection in hyponatremic patients has the potential to improve survival compared to non-administration, but drawing a valid conclusion is difficult due to the low level of evidence.
Desmopressin is an antidiuretic hormone that binds to the V2 receptor in the collecting duct and increases the expression of aquaporin channels to increase water reabsorption of urine passing through the collecting duct. A number of studies found that administration of desmopressin can prevent rapid correction of hyponatremia or stabilize SNa correction rate through water reabsorption if it has already been rapidly corrected. The European guideline recommended that 2 µg of intravenous desmopressin be given at intervals of 8 hours or more to prevent rapid correction (grade of recommendation 1D). In addition, they also recommend injecting 10 mL/kg of electrolyte-free water (dextrose solution) for 1 hour in consideration of urine volume and fluid balance (grade of recommendation 1D). However, there have been no prospective studies on this recommendation. In two retrospective observational studies cited in the guidelines, SNa concentration was corrected using desmopressin or electrolyte-free water to the target of 12 mmol/L within 24 hours and less than 18 mmol/L within 48 hours when overcorrection occurred [50]. In one of these retrospective studies, the proactive strategies in which hypertonic fluid and desmopressin were concurrently administered increased SNa concentration stably, and SNa concentration was maintained within the target range for 24 and 48 hours [51]. However, the quality of the studies included in the guidelines varied, the criteria for classification of hyponatremia among the study subjects varied, and there was no comparative study in which patients not using desmopressin were included as a control group. Eighty patients using desmopressin were classified into three strategies in one SR of desmopressin use for hyponatremia in 2015 [52]. The proactive strategy was based on initial SNa concentration, with desmopressin administered before concentration changes of SNa. In the reactive strategy, desmopressin was administered according to an increase in the concentration of SNa or urine output. In the rescue strategy, desmopressin was administrated to re-lower SNa concentration in case of overcorrection. However, final conclusions could not be drawn on the optimal strategy for administration of desmopressin for hyponatremia due to limitations of the study design and sample size.
In this guideline, we evaluated one SR study and three observational studies on whether the administration of desmopressin for hyponatremia has additional benefit in the prevention of overcorrection, complications (ODS), and prognosis (survival to discharge) compared to the non-administered group [50,52–54]. As a result of our analysis, overcorrection prevention did not differ significantly when comparing the group with and without use of desmopressin (proactive and reactive strategies). When the desmopressin use group and the non-desmopressin group were compared, including proactive, reactive, and rescue therapy, the incidence of ODS was higher in the group using desmopressin, but ODS occurred in only one or two cases, and there was a possibility of selection bias. When comparing the survival to discharge of the groups administered and not administered desmopressin (proactive, reactive and rescue strategies), survival rate was significantly higher in the desmopressin use group. However, a larger sample size and prospective studies are needed to determine the optimal strategy for desmopressin administration in hyponatremia.
5) Special situations 1. Treatment of hyponatremia in patients with brain lesions
Recommendation 8
We consider it reasonable that treatment with hypertonic or isotonic saline infusion, oral sodium chloride, or fludrocortisone for the correction of hypoosmolar hyponatremia should be individualized among patients with cerebral diseases (E).
Remarks:
1. The causes of hypoosmolar hyponatremia among patients with cerebral diseases are diverse, and include SIAD, CSW, and insufficient cortisol secretion.
2. There is insufficient evidence that hypoosmolar hyponatremia in patients with cerebral diseases can be effectively corrected with a crystalloid solution, including normal saline.
Hyponatremia occurs very frequently in patients with various cerebral diseases such as traumatic brain injury, intracranial or subarachnoid hemorrhage, brain tumor, brain surgery, cerebral infarction, and meningitis. The incidence of hyponatremia in traumatic brain injury patients has been reported to be 27% to 51% [55,56], 40% to 45% in cerebral infarction patients [57], 14% to 63% in subarachnoid hemorrhage [57,58], and 15% to 20% of brain tumor patients [59]. Various factors such as SIAD, CSW, and insufficient secretion of cortisol are major causes of hyponatremia in cerebral diseases. The most common cause of hyponatremia in patients with cerebral disease is SIAD, accounting for approximately 62%, and volume deficit or CSW accounted for about 30% [59].
Concomitant hyponatremia in patients with cerebral disease is closely related to the deterioration of patient condition. Therefore, appropriate treatment depending on the cause of hyponatremia is highly recommended [2]. However, in a clinical setting, it is not easy to accurately determine the cause based on patient volume status and it may require several hours or days to complete diagnostic tests and evaluations to determine the cause. Therefore, the CPG Committee sought to suggest appropriate treatment guidelines for hypoosmolar hyponatremia in patients with various cerebral diseases. We searched Ovid MEDLINE, Embase, Cochrane Library, and KMbase, and found a total of 72 research papers through additional manual searches. We selected 66 documents excluding duplicates and reviewed 13 original texts. We could not find any documents that suitably addressed this key question. Therefore, an expert consensus was made by organizing the results of related research with the existing CPGs.
The American guideline suggested that in the case of hyponatremia in patients with cerebral disease, treatment such as normal saline, oral salt supplementation, hypertonic saline, and fludrocortisone may be considered [2]. In general, treatment guidelines recommend water restriction or hypertonic saline depending on the severity of hyponatremia in SIAD. In addition, volume depletion is common in patients with various cerebral diseases [60]. In particular, volume deficit (body fluid deficiency) accompanying CSW can result in hyponatremia. The occurrence of cerebral infarction and other neurological complications increases when water restriction is implemented in patients with cerebral disease [61,62]. Therefore, in the case of hyponatremia accompanying these cerebral diseases, clinicians should avoid volume depletion through water restriction [63].
Hyponatremia accompanied by neurological symptoms related to hyponatremia can be corrected through hypertonic saline to prevent the progression of neurological complications. However, it should be treated cautiously by controlling the rate of correction to avoid overcorrection in accordance with the general principles of hyponatremia correction rate. Asymptomatic hypoosmolar hyponatremia occurring in patients with cerebral diseases can be initially corrected by preferentially using isotonic crystalloid solution including normal saline, unless volume depletion is clearly excluded by clinical judgment. In the case of asymptomatic hypoosmolar hyponatremia that does not improve despite administering isotonic crystalloid solution such as normal saline, evaluation and tests for differential diagnosis may be performed, and concomitant salt supplementation such as hypertonic saline or oral salt may be considered. In the case of CSW, hyponatremia can be corrected with a mineralocorticoid such as fludrocortisone. Hasan et al. [64] demonstrated the effectiveness of fludrocortisone treatment for the prevention of renal salt excretion and volume status decrease in 91 patients with subarachnoid hemorrhage, which is commonly accompanied by CSW, through a RCT. Misra et al. [65] conducted a RCT on 38 hyponatremic patients with tuberculous meningitis due to CSW and showed that fludrocortisone treatment can correct hyponatremia earlier than normal saline. Further evidence is needed for specific recommendations in hyponatremia patients with cerebral diseases.
6) Special situations 2. Selection of maintenance fluid to prevent hyponatremia in children aged ≤18 years
Recommendation 9
1. To prevent hyponatremia, we recommend the administration of isotonic fluids as maintenance fluid therapy in hospitalized pediatric patients over 1 month and under 18 years of age (A, high).
2. There are insufficient data to make a recommendation regarding administrating isotonic fluids as maintenance fluid therapy to prevent hyponatremia in neonates because of the risk of hypernatremia (I, moderate).
Remarks:
1. In maintenance fluid therapy for children and adolescents over 1 month and under 18 years of age, the administration of isotonic fluid is effective for preventing the development of hyponatremia and has similar risk of hypernatremia compared to the administration of hypotonic fluids.
2. In maintenance fluid therapy for neonates less than 1 month old, the administration of isotonic fluid is effective for preventing the development of hyponatremia and leads to a higher risk of developing hypernatremia compared to the administration of hypotonic fluids.
Traditionally, hypotonic solutions based on the Holliday-Segar formula have been used as maintenance fluids in hospitalized pediatric patients under the age of 18 years. However, the development of hyponatremia associated with hypotonic solution administration and related neurologic complications and death have been continuously reported. In addition, children are more likely to develop severe symptoms associated with hyponatremia because the brain is relatively large compared to the skull in children. Consequently, there has been controversy over the composition of optimal maintenance fluid. In 2018, the American Academy of Pediatrics recommended an isotonic solution as a maintenance fluid for pediatric patients over 1 month old by integrating evidence from 17 RCTs and seven SRs (grade of recommendation 1A) [66]. In the 2020 revised NICE (National Institute for Health and Care Excellence) guidelines, isotonic solutions were recommended as maintenance fluids in children, including term neonates 8 days of age or older [67]. However, RCT studies have shown inconsistent results.
In this guideline, we performed a meta-analysis by synthesizing 18 RCTs (16 RCTs for children over 1 month and two RCTs for newborns) [68–85] and seven SRs [86–88]. We sought to examine whether the administration of isotonic fluid compared to hypotonic fluids reduced the incidence of hyponatremia without increasing the risk of hypernatremia during maintenance fluid therapy in pediatric patients including newborns. In 18 RCTs, normal saline or Ringer’s lactate solution as an isotonic solution and 0.20% to 0.45% saline as a hypotonic solution were administered to hospitalized pediatric patients. In most studies, 5% dextrose solution was added to the maintenance fluid. A total of 3,231 patients were included in 16 RCT studies of children 1 month and older, including patients who were hospitalized for surgery or were admitted to the intensive care unit, and those who were hospitalized for pneumonia or central nervous system infection. Of these, isotonic solutions were used in 1,608 patients and hypotonic solutions were used in 1,623 patients as maintenance fluid. The incidence of hyponatremia in patients using isotonic solution as maintenance treatment was significantly lower than in the group using hypotonic solution as maintenance treatment (OR, 0.32; 95% CI, 0.24–0.43; p < 0.001). Although hypernatremia was increased in patients administered isotonic solutions in some studies [68–71,74,78], there was no significant difference in a meta-analysis between isotonic fluid and hypotonic fluid (OR, 1.67; 95% CI, 0.92–3.04; p = 0.09). In two non-RCTs, the incidence of hyponatremia had a tendency to be low in patients administered isotonic fluids; however, this was not statistically significant (OR, 0.54; 95% CI, 0.28–1.02; p = 0.05), and the incidence of hypernatremia in patients receiving isotonic fluids was not significantly different from that in patients receiving hypotonic fluids (OR, 1.25; 95% CI, 0.73–2.13; p = 0.58). Two RCTs enrolled a total of 144 neonates, including premature babies aged 34 weeks or older and full-term neonates. Of these, 73 patients received isotonic fluid and 71 received 0.15% to 0.20% hypotonic fluid. These studies reported a significantly lower incidence of hyponatremia in patients receiving isotonic fluids (OR, 0.11; 95% CI, 0.03–0.35; p < 0.001) than in patients receiving hypotonic fluids. However, the incidence of hypernatremia was significantly higher in patients receiving isotonic fluids than in patients receiving hypotonic fluids (OR, 8.24; 95% CI, 1.84–36.91; p < 0.001) [73,77].
Notes
Access to the full-text version
The full-text version of this clinical practice guideline is available on the Korean Society of Nephrology website (https://doi.org/10.23876/j.krcp.33.666).
Conflict of interest
All authors have no conflicts of interest to declare.