| Kidney Res Clin Pract > Volume 31(3); 2012 > Article |
|
Abstract
Background
The variable clinical and histopathological manifestations of immunoglobulin A nephropathy (IgAN) make it difficult to predict disease progression. A recent study showed that hyperuricemia, a condition common in hypertension and vascular disease, may contribute to renal dysfunction and histological changes including renal arteriosclerosis, tubular atrophy, and interstitial fibrosis. Herein, we investigated the clinical significance of uric acid level at the time of biopsy, as a marker of IgAN progression.
Methods
We included 193 patients with biopsy-proven IgAN. Renal disease progression was defined as serum creatinine elevation above 1.2 mg/dL or over 20% elevation from baseline. Hyperuricemia was defined as a serum uric acid level ≥7.3 mg/dL in men and ≥5.3 mg/dL in women, which were 1 standard deviation above the mean value in the normal subjects.
Results
The hyperuricemia group (n=50) had higher blood pressure, body mass index, and serum creatinine, and a greater amount of proteinuria and a lower glomerular filtration rate than the nonhyperuricemia group (n=143). Hyperuricemia increased the risk of IgAN progression (odds ratio, 4.53; 95% confidence interval, 1.31–15.66). The disease progression group (n=26) had a greater frequency of hyperuricemia, hypertension, and nephrotic range proteinuria than the nonprogression group (n=119). The renal survival analysis showed that the hyperuricemia group had a higher rate of IgAN disease progression.
Keywords
Hyperuricemia, Immunoglobulin A nephropathyImmunoglobulin A nephropathy (IgAN) is the most common chronic glomerulonephritis worldwide [1]. The course of IgAN is variable, with 10%–20% of patients developing end-stage renal disease in the first 10 years after the diagnosis [2]. Early detection and intervention for adjustable risk factors may reduce or slow the rate of progression of chronic renal disease. The risk factors associated with poor prognosis are renal insufficiency, hypertension, and proteinuria at the time of diagnosis [3]. Recent studies suggest that uric acid is associated with IgAN progression [4], [5].
High serum uric acid levels may reflect a decrease in renal blood flow and early hypertensive nephrosclerosis. Serum uric acid may play a pathologic role in renal vasoconstriction, endothelial dysfunction, inflammatory response, oxidative stress, and the disturbances in autoregulation that occur with acute renal failure [6]. Recently, the reassessment of the role of hyperuricemia suggests its direct pathogenicity as well as a marker for other associated risk factors [7], [8], [9], [10].
The aim of the present study was to evaluate the association between uric acid levels at the time of IgAN diagnosis and renal prognosis in patients with biopsy-proven IgAN.
This study included all the patients with IgAN diagnosed at the Soonchunhyang University Cheonan Hospital between January 1999 and December 2005. A renal biopsy specimen was considered adequate if it contained 4 or more glomeruli. IgAN was defined as glomerulonephritis with predominant IgA deposition in the glomerular mesangium. 193 patients (103 men [53.4%] and 90 women [46.6%]) fulfilled this criterion. The median age at the time of renal biopsy was 34 years (range 14–71). The Hospital’s Investigational Review Board approved this study and all participants provided written informed consent. The clinical data were collected by retrospective review of the medical record system of the Hospital.
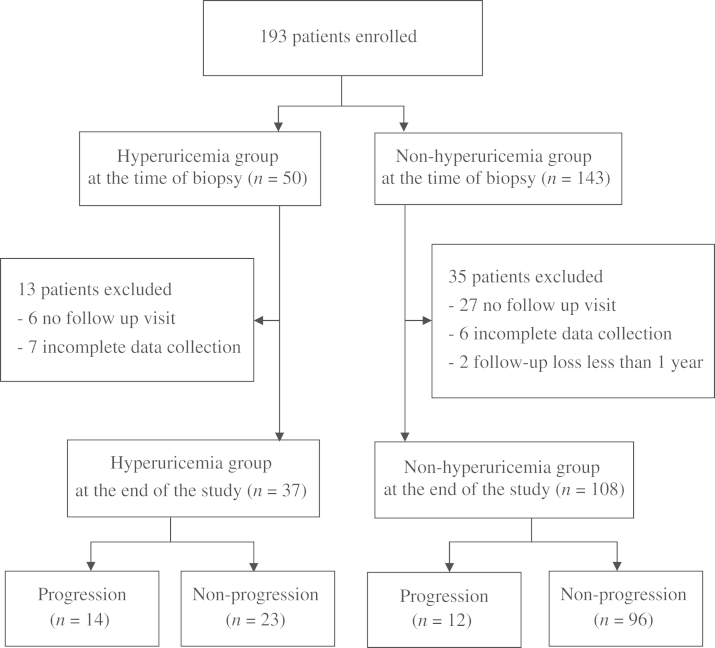
Systemic lupus erythematosus, liver cirrhosis, or the typical picture of Henoch–Schönlein purpura was not observed in our cases. Of the 193 patients (hyperuricemia, n=50; nonhyperuricemia, n=143) enrolled in the study at the time of renal biopsy, 48 (24.9%) were excluded: 33 did not attend follow-up visits, 13 had incomplete laboratory data, and 2 were followed for <1 year. Thus, 145 patients were included in the analysis (hyperuricemia, n=37; nonhyperuricemia, n=108; Fig. 1). The median follow-up time after renal biopsy was 5.8 years (range 1.2–10). All the clinical parameters were measured at the time of renal biopsy. Data on medication, diabetes mellitus, body mass index (BMI), blood pressure (BP), 24-h urinary protein excretion, serum lipid profile, and serum uric acid level at the time of renal biopsy were recorded. The definition of hypertension was the use of antihypertensive medication at the time of renal biopsy or a systolic BP >140 mmHg and/or diastolic BP >90 mmHg as measured during hospitalization for renal biopsy. By this definition, 40 patients had hypertension. Nine patients had diabetes mellitus (non–insulin-dependent diabetes mellitus). The pathology grading system was determined according to Lee [11]. Hypercholesterolemia and hypertriglyceridemia were defined as serum cholesterol >250 mg/dL and serum triglyceride >200 mg/dL, respectively.
From January 2002 to May 2007, the 7,354 people who presented for a medical check-up at the health promotion center of Soonchunhyang University Cheonan Hospital were enrolled as a control group to define hyperuricemia. Of them, 1,109 cases with hematuria, proteinuria, hypertension, or diabetes mellitus were excluded. The uric acid level (mean±SD) of this control group (n = 6,245) was 5.24±1.43 mg/dL, with men (n=3,509) having mean values of 6.02±1.27 mg/dL and women (n=2,736), 4.32±0.97 mg/dL. Hyperuricemia was defined as a serum uric acid level ≥7.3 mg/dL in men or ≥5.3 mg/dL in women. These cut off points are 1 standard deviation above the mean values in the normal control subjects.
The initial measurement of serum creatinine was obtained at the time of the renal biopsy. The serum creatinine measured at the last follow-up visit was used when defining IgAN progression. Serum creatinine values were considered normal if they were ≤1.2 mg/dL. IgAN progression during follow-up was defined as elevation of the serum creatinine above the normal level or a >20% increase from the baseline level (in patients who had elevated creatinine at the time of biopsy). Serum creatinine values were measured at approximately 1-year intervals during the follow-up. These values were used when studying the time interval in years until impaired renal function developed; this interval was used in renal survival curve analysis in relation to hyperuricemia. Urine protein excretion was measured in a 24-h urine collection. Proteinuria and nephrotic range proteinuria were defined as protein excretion ≥1 g/day and ≥3.5 g/day, respectively.
Data are presented as the mean (SD) values for continuous variables and as frequency (percentage) for categorical variables. A P value <0.05 was considered statistically significant. The statistical analysis was performed with the SPSS program for Windows (version 14.0; SPSS, Inc., Chicago, Illinois, USA). The inter-group differences were compared with the Student t test for continuous variables and the Chi-square test for categorical variables. Survival analysis for stable renal function related to hyperuricemia was carried out by the Kaplan–Meier survival curve. Differences between survival curves were tested by the log-rank test. Multiple logistic regression analysis was used to determine the factors affecting IgAN progression. The strength of the association between uric acid and IgAN progression was expressed as odds ratio (OR).
The hyperuricemia group had higher systolic and diastolic BP, BMI, serum creatinine, serum cholesterol, and triglycerides (Table 1). In addition, patients with hyperuricemia showed class IV and V renal lesions and lower glomerular filtration rate (GFR; <60 mL/min/1.73 m2) and proteinuria more frequently than patients without hyperuricemia at the time of renal biopsy (Table 1). Univariate analysis between GFR and hyperuricemia showed that hyperuricemia increased the risk of GFR<60 mL/min/1.73 m2 by 6.14-fold [95% confidence interval (CI) 2.69–14.03]. After adjustments for age, gender, hypertension, BMI, hypercholesterolemia, and hypertriglyceridemia, the risk was still increased by 4.20-fold (95% CI 1.53–11.52; Table 2).
Among 145 patients, 121 (81%) had normal serum creatinine levels and 24 (19%) had elevated levels at the time of the renal biopsy. IgAN progression was found in 8 of the 24 patients (33.3%) with elevated serum creatinine at biopsy. Patients with progression had initially higher levels of systolic and diastolic BP, uric acid, and triglycerides, and a higher frequency of proteinuria and nephrotic range proteinuria (Table 3). The serum creatinine was normalized in 9 of these 24 (37.5%) patients, but remained elevated without a further increase over 20% in 7 (29.1%). Thus, 26 (17.9%) of the study patients had IgAN progression according to the definition in this study. In 24 of these 26 patients, the last measured serum creatinine was >1.5 mg/dL. The serum creatinine increased from 0.8 to 1.3 mg/dL and from 0.9 to 1.4 mg/dL in 2 of the 26 patients. End stage renal disease (requiring dialysis) developed in 11 patients (5.5%).
The serum uric acid level at the time of renal biopsy was significantly higher in patients who progressed than those who did not (Table 3) and hyperuricemia was associated with a poor prognosis (Table 4). Hyperuricemia increased the risk of IgAN progression by 4.87 (range 1.99–11.92) in the unadjusted analysis. After adjustment for age, gender, hypertension, hypertriglyceridemia, hypercholesterolemia, BMI, and proteinuria, patients with hyperuricemia still had a significantly increased risk of IgAN progression (mean 4.53, range 1.31–15.66; Table 4).
The renal survival curves differed significantly depending on the presence of hyperuricemia (Fig. 2).
Class IV and V renal lesions, hypertension, and proteinuria were significantly associated with a poor prognosis (Table 3). A significant relationship was not found between hyperuricemia and proteinuria.
Hyperuricemia, which is a predictor of coronary heart disease, stroke, and atherosclerosis, may also have a direct pathogenic role in the deterioration of renal function [7], [8], [9], [10], [12], [13], [14], [15]. Many clinical studies have shown significant correlations between serum uric acid and tubular atrophy, interstitial fibrosis and inflammation, proteinuria, and glomerulosclerosis [7], [9], [10]. Although the underlying mechanisms remain undetermined, hyperuricemia at the time of renal biopsy was found to be a predictor of poor prognosis in patients with normal renal function at the time of biopsy [4].
Numerous studies have assessed the risk factors for progression of renal insufficiency in IgAN. Hypertension, an elevated serum creatinine concentration, severe proteinuria, older age, male gender, and the absence of macroscopic hematuria were found to be independent risk factors [3], [24]. Recent studies have shown that hyperuricemia is also an important risk factor for IgAN progression, which is related to the central role of hyperuricemia in tubulointerstitial damage [3], [4], [5].
Factors such as volume depletion, alcohol intake, and a high purine diet may cause hyperuricemia [10], [16]. Furthermore, a decreased GFR may result in decreased uric acid excretion in the urine, depending on the degree of gastrointestinal excretory compensation, and this may cause hyperuricemia [17], [18]. However, whether hyperuricemia increases the risk of renal progression or is associated with a decrease in GFR is not entirely clear. Hyperuricemia was an independent risk factor for IgAN progression in a study of patients with normal renal function [4]. In this study, subgroup analysis of patients with normal renal function at diagnosis of IgAN showed that hyperuricemia has a tendency to increase the risk of IgAN progression. Furthermore, the presence of hyperuricemia significantly increased the risk for progression of IgAN in the whole patients in the multiple regression analysis.
The presence of hyperuricemia is an independent predictor for the development of hypertension [1], [2], and hypertension is a risk factor for IgAN progression and virtually all other renal diseases. At the diagnosis of IgAN, hypertension was observed in 6% to 49% of patients [3]; in this study, the frequency of hypertension was 20.7%. Hypertension was more common in the hyperuricemia group than in the nonhyperuricemia group (32% vs. 16.8%, P=0.027). Multiple logistic regression analysis showed that hypertension significantly increased the risk of IgAN progression and hyperuricemia.
Proteinuria appears to be an independent clinical risk factor predictive of a progressive course in patients with IgAN. Generally, urinary protein excretion >1 g/day is known to increase the risk of poor renal outcome [3], [19], [20], [21]. In this study, 37.8% (73/193) of patients had proteinuria ≥1 g/day and patients with hyperuricemia were more likely to have proteinuria than those without hyperuricemia (56.0% vs. 31.5%, respectively; P<0.01). Furthermore, proteinuria was an independent risk factor for IgAN progression in the multiple regression analysis.
The association between the initial uric acid level and the longitudinal change in proteinuria was evaluated. However, significant associations were not found between hyperuricemia and the changes in the amount of proteinuria.
Hyperuricemia has been associated with several components of the metabolic syndrome, including hypertension, glucose intolerance, high BMI, and obesity. Obesity with hypertension or hyperlipidemia may accelerate renal damage [22] and promote proteinuria in healthy men [23]. Hypertriglyceridemia and a high BMI are potential independent risk factors for IgAN progression. In the present study, a high BMI and hypertriglyceridemia were common in patients with hyperuricemia, and these patients had an increased risk of IgAN progression in the univariate analysis. However, the multiple regression analysis did not show a significant association.
This study had several limitations. First, the serum uric acid level was measured on only one occasion, resulting in a possible underestimation of the strength of its association with IgAN progression. An average value, determined by multiple measurements, would yield greater differences in the frequency of IgAN progression associated with hyperuricemia. Second, in addition to a decrease in the GFR, factors such as volume depletion, alcohol intake, and a high purine diet are causes of hyperuricemia [10], [16]. Unfortunately, this study did not evaluate these factors. Third, the current results do not definitively show that uric acid itself caused the disease and/or its progression because of the observational study design.
We conclude that, in addition to various risk factors such as hypertension, proteinuria, and hyperlipidemia, hyperuricemia at the time of IgAN diagnosis is an important and independent risk factor for IgAN progression.
Acknowledgments
The work was supported by the National Research Foundation of Korea (NRF) grant funded by the Ministry of Education, Science and Technology (MEST) of Korea Government (2010-0005071).
References
1. Julian B.A., Waldo F.B., Rifai A., Mestecky J.. IgA nephropathy, the most common glomerulonephritis worldwide. A neglected disease in the United States? Am J Med 84:1988;129–132.
2. D'Amico G.. Natural history of idiopathic IgA nephropathy and factors predictive of disease outcome. Semin Nephrol 24:2004;179–196.


3. D’Amico G.. Natural history of idiopathic IgA nephropathy: role of clinical and histological prognostic factors. Am J Kidney Dis 36:2000;227–237.


4. Syrjänen J., Mustonen J., Pasternack A.. Hypertriglyceridaemia and hyperuricaemia are risk factors for progression of IgA nephropathy. Nephrol Dial Transplant 15:2000;34–42.

5. Ohno I., Hosoya T., Gomi H., Ichida K., Okabe H., Hikita M.. Serum uric acid and renal prognosis in patients with IgA nephropathy. Nephron 87:2001;333–339.



6. Ejaz A.A., Mu W., Kang D.H., Roncal C., Sautin Y.Y., Henderson G., Tabah-Fisch I., Keller B., Beaver T.M., Nakagawa T., Johnson R.J.. Could uric acid have a role in acute renal failure? Clin J Am Soc Nephrol 2:2007;16–21.


7. Kang D.H., Nakagawa T., Feng L., Watanabe S., Han L., Mazzali M., Truong L., Harris R., Johnson R.J.. A role for uric acid in the progression of renal disease. J Am Soc Nephrol 13:2002;2888–2897.


8. Feig D.I., Nakagawa T., Karumanchi S.A., Oliver W.J., Kang D.H., Finch J., Johnson R.J.. Hypothesis: Uric acid, nephron number, and the pathogenesis of essential hypertension. Kidney Int 66:2004;281–287.


9. Johnson R.J., Kivlighn S.D., Kim S.G., Suga S., Fogo A.B.. Reappraisal of the pathogenesis and consequences of hyperuricemia in hypertension, cardiovascular disease, and renal disease. Am J Kidney Dis 33:1999;225–234.


10. Johnson R.J., Kang D.H., Feig D., Kivlighn S., Kanellis J., Watanabe S., Tuttle K.R., Rodriguez-Iturbe B., Herrera-Acosta J., Mazzali M.. Is there a pathogenetic role for uric acid in hypertension and cardiovascular and renal disease? Hypertension 41:2003;1183–1190.


11. Lee S.M., Rao V.M., Franklin W.A., Schiffer M.S., Aronson A.J., Spargo B.H., Katz A.I.. IgA nephropathy: morphologic predictors of progressive renal disease. Hum Pathol 13:1982;314–322.


12. Selby J.V., Friedman G.D., Quesenberry C.P. Jr. Precursors of essential hypertension: Pulmonary function, heart rate, uric acid, serum cholesterol, and other serum chemistries. Am J Epidemiol 131:1990;1017–1027.


13. Jossa F., Farinaro E., Panico S., Krogh V., Celentano E., Galasso R., Mancini M., Trevisan M.. Serum uric acid and hypertension: the Olivetti heart study. J Hum Hypertens 8:1994;677–681.

14. Fang J., Alderman M.H.. Serum uric acid and cardiovascular mortality. The NHANES I epidemiologic follow-up study, 1971–1992. National Health and Nutrition Examination Survey. JAMA 283:2000;2404–2410.


15. Iseki K., Ikemiya Y., Inoue T., Iseki C., Kinjo K., Takishita S.. Significance of hyperuricemia as a risk factor for developing ESRD in a screened cohort. Am J Kidney Dis 44:2004;642–650.


16. Johnson R.J., Rideout B.A.. Uric acid and diet - Insights into the epidemic of cardiovascular disease. N Engl J Med 350:2004;1071–1073.


17. Siu Y.P., Leung K.T., Tong M.K., Kwan T.H.. Use of allopurinol in slowing the progression of renal disease through its ability to lower serum uric acid level. Am J Kidney Dis 47:2006;51–59.


18. Vaziri N.D., Freel R.W., Hatch M.. Effect of chronic experimental renal insufficiency on urate metabolism. J Am Soc Nephrol 6:1995;1313–1317.


19. Radford M.G. Jr, Donadio J.V. Jr, Bergstralh E.J., Grande J.P.. Predicting renal outcome in IgA nephropathy. J Am Soc Nephrol 8:1997;199–207.


20. Frimat L., Briancon S., Hestin D., Aymard B., Renoult E., Huu T.C., Kessler M.. IgA nephropathy: Prognostic classification of end-stage renal failure. L'Association des Néphrologues de l'Est. Nephrol Dial Transplant 12:1997;2569–2575.

21. Donadio J.V., Bergstarlh E.J., Grande J.P., Rademcher D.M.. Proteinuria patterns and their association with subsequent end-stage renal disease in IgA nephropathy. Nephrol Dial Transplant 17:2002;1197–1203.


22. Sasatomi Y., Tada M., Uesugi N., Hisano S., Takebayashi S.. Obesity associated with hypertension or hyperlipidemia accelerated renal damage. Pathobiology 69:2001;113–118.



Figure 2
Cumulative renal survival curves in the non-hyperuricemia and the hyperuricemia groups (P<0.001).
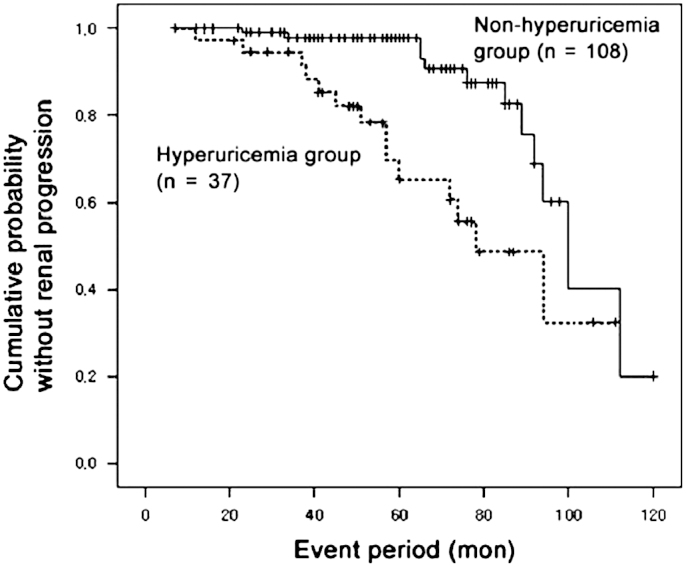
Table 1
Clinical characteristics of IgAN patients with or without hyperuricemia at the time of renal biopsy
| Hyperuricemia⁎ (n = 50) | Nonhyperuricemia (n = 143) | P | |
|---|---|---|---|
| Sex, men, n (%) | 25 (50%) | 78 (54.5%) | 0.6† |
| Age | 34.94±12.14 | 33.34±13.69 | 0.5 |
| DM, n (%) | 2 (4.0%) | 8 (5.6%) | 1.000† |
| Hypertension n (%) | 16 (32.0%) | 24 (16.8%) | 0.03† |
| Systolic BP (mmHg) | 127.60±13.33 | 120.94±15.63 | 0.008 |
| Diastolic BP (mmHg) | 81.20±9.18 | 76.75±10.35 | 0.008 |
| BMI | 25.38±4.16 | 22.76±2.94 | 0.000 |
| Albumin (g/dL) | 3.84±0.64 | 3.82±0.66 | 0.8 |
| Blood urea nitrogen (mg/dL) | 19.84±13.07 | 13.55±4.41 | <0.001 |
| Creatinine (mg/dL) | 1.46±1.27 | 0.98±0.27 | <0.001 |
| Initial GFR (ml/min/1.73 m2) | 69.59±29.27 | 89.90±23.14 | <0.001 |
| Uric acid (mg/dL) | 7.66±1.66 | 4.92±1.23 | <0.001 |
| Cholesterol (mg/dL) | 174.53±96.96 | 119.86±64.90 | <0.001 |
| Triglyceride (mg/dL) | 204.98±48.97 | 175.15±51.43 | <0.001 |
| Hypercholesterolemia, n (%) | 10 (20.0%) | 9 (6.3%) | 0.010† |
| Hypertriglyceridemia, n (%) | 27 (54%) | 26 (18.2%) | <0.001† |
| 24-h protein (mg/d) | 1585±1643 | 1386±2679 | 0.6 |
| Proteinuria (>1.0 g/d), n (%) | 28 (56.0%) | 45 (31.5%) | 0.004† |
| Proteinuria (>3.5 g/d), n (%) | 7 (14.0%) | 13 (9.2%) | 0.4† |
| Pathologic grade IV/V‡, n (%) | 14 (28%) | 7 (4.9%) | <0.001† |
SI conversion factors: values were multiplied by 10 to convert albumin to g/L; values were multiplied by 0.357 to convert blood urea nitrogen to mmol/L; values were multiplied by 88.4 to convert creatinine to μmol/L; values were multiplied by 59.48 to convert uric acid to μmol/L; values were multiplied by 0.02586 to convert cholesterol to mmol/L; and values were multiplied by 0.01129 to convert triglyceride to mmol/L.
‡ The pathologic grading system was determined according to Lee [11].
Table 2
Hyperuricemia for the risk of GFR<60 ml/min/1.73 m2
| Odds ratio (95% confidence interval) for GFR<60 ml/min/1.73 m2 in hyperuricemia | |
|---|---|
| Model 1 | 6.14 (2.69–14.03) |
| Model 2 | 6.76 (2.83–16.10) |
| Model 3 | 4.20 (1.53–11.52) |
Table 3
Basal clinical characteristics of progression and nonprogression groups
| Progression group (n=26) | Nonprogression group (n=119) | P | |
|---|---|---|---|
| Sex, men, n (%) | 61.5% (16) | 52.1% (62) | 0.5⁎ |
| Age | 35.58±13.58 | 34.03±13.21 | 0.6 |
| DM, n (%) | 1 (3.8%) | 6 (5.0%) | 1.000⁎ |
| Hypertension, n (%) | 11 (42.3%) | 21 (17.6%) | 0.009⁎ |
| Hyperuricemia, n (%) | 14 (53.8%) | 23 (19.3%) | 0.001⁎ |
| Systolic BP (mmHg) | 131.15±16.57 | 120.55±14.87 | 0.002 |
| Diastolic BP (mmHg) | 83.46±7.45 | 76.60±10.31 | 0.002 |
| BMI | 24.45±4.78 | 23.20±3.36 | 0.1 |
| Albumin (g/dL) | 3.39±0.65 | 3.89±0.61 | <0.001 |
| BUN (mg/dL) | 18.52±6.73 | 14.04±4.99 | <0.001 |
| Creatinine (mg/dL) | 1.30±0.66 | 1.00±0.30 | <0.001 |
| Initial GFR (ml/min/1.73 m2) | 73.44±29.92 | 86.79±23.71 | 0.01 |
| Uric acid (mg/dL) | 6.85±1.76 | 5.36±1.61 | <0.001 |
| Cholesterol (mg/dL) | 155.44±91.07 | 126.99±68.64 | 0.08 |
| Triglyceride (mg/dL) | 210.00±61.14 | 178.81±51.20 | 0.007 |
| Hypercholesterolemia, n (%) | 6 (23.1%) | 8 (6.7%) | 0.02⁎ |
| Hypertriglyceridemia, n (%) | 13 (50.0%) | 28 (23.5%) | 0.01⁎ |
| 24-h urine protein (mg/day) | 3156±2752 | 1225±2610 | 0.001 |
| Proteinuria (>1.0 g/d), n (%) | 19 (73.1%) | 38 (31.9%) | <0.001⁎ |
| Proteinuria (>3.5 g/d), n (%) | 9 (34.6) | 10 (8.4%) | 0.001⁎ |
| Pathologic grade IV/V†, n (%) | 12 (46.2) | 4 (3.4%) | <0.001⁎ |
† The pathologic grading system was determined according to Lee [11].



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print
















