| Kidney Res Clin Pract > Volume 38(4); 2019 > Article |
|
Abstract
Background
Previous studies have recommended a 2- to 5-year waiting time prior to kidney transplantation (KT) in patients with end-stage renal disease (ESRD) and symptomatic renal cell carcinoma (RCC) and no delay for incidental early-stage RCC. Data on Asian KT recipients are unavailable.
Methods
This is a Korean single-center retrospective study on 35 KT recipients with ESRD and RCC. Patients were classified into two groups: early KT (KT performed within 1 year after nephrectomy for RCC, including KT with simultaneous nephrectomy) and delayed KT (KT performed over than 1 year after nephrectomy for RCC). Patient survival, graft survival, and cancer recurrence were compared between both groups.
Results
There were no statistically significant differences in patient survival (P = 0.388), graft survival (P = 0.317), or graft rejection rate (P = 0.207) between the early and delayed KT groups. Additionally, there were no differences in pathological characteristics or RCC stage other than cancer histology: acquired cystic disease-associated RCC (47.4%) was the most common RCC type in the early KT group, whereas clear cell type (62.5%) was the most common RCC type in the delayed KT group. No RCC recurrence was observed.
The incidence of kidney cancer increases in patients with end-stage renal disease (ESRD) on chronic dialysis [1,2], and renal cell carcinoma (RCC) is the predominant type [3]. The incidence of RCC has been reported to be higher in patients with ESRD than in the general population [4]. Despite this higher incidence, in several studies, cancer-specific mortality has been reported to be lower in patients with ESRD than in the general population [5ŌĆō7]. Hashimoto et al. attributed better prognosis of RCC in patients with ESRD on hemodialysis to younger age, smaller tumor size, and early tumor stage [7]. RCC in patients with ESRD is often incidentally found without specific symptoms, and these patients typically have a comparatively favorable outcome [8ŌĆō10]. One previous study showed that RCC detected by screening had improved patient survival compared to RCC presenting with symptoms in patients on dialysis [11].
As kidney transplant (KT) recipients typically receive immunosuppressive therapy, cancer recurrence after KT is a clinically important issue. Therefore, there are guidelines regarding waiting time for KT in patients with ESRD and RCC [12]. Previous studies have suggested a waiting period of 2 to 5 years before KT in patients with symptomatic RCC and no delay in patients with incidental early-stage RCC [13ŌĆō15], which is sometimes diagnosed during the pre-KT workup.
Recently, a multicenter study from France reported on RCC recurrence after KT [16], and other studies have suggested racial differences in the histology and prognosis of RCC [17,18]. However, data on Asian KT recipients with RCC are insufficient. Accordingly, this study aimed to identify the clinical characteristics of KT recipients with RCC at our center and to analyze clinical outcomes to determine the appropriate waiting time for KT in this patient population.
We conducted a single-center retrospective observational study at the Asan Medical Center (AMC), Seoul, Republic of Korea. Approval was obtained from the Institutional Review Board of AMC (approval number: 2018-0826). Since this is a retrospective study, written informed consent was waived by the IRB. We reviewed the medical records of patients diagnosed with RCC and treated before KT among recipients who underwent KT between 1990 and 2017. Patients were classified into two groups: early KT (KT performed within 1 year after nephrectomy for RCC, including KT with simultaneous nephrectomy) and delayed KT (KT performed > 1 year after nephrectomy for RCC).
We investigated demographic data, such as sex, age at time of KT, underlying diseases before transplantation, cause of ESRD, dialysis status, and follow-up duration after KT. RCC data included cancer staging, histopathology, and time from nephrectomy to KT. KT data included donor type, donor age, human leukocyte antigen (HLA) mismatch, ABO incompatibility, and maintenance immunosuppressive therapy used, including mammalian target of rapamycin inhibitors. Clinical outcomes included patient survival, graft survival, graft rejection rate, and RCC recurrence. Acute rejection was defined using the Banff classification and confirmed by allograft biopsy when clinically suspected because of increased serum creatinine levels. Graft failure was defined as the initiation of dialysis therapy or second KT. RCC staging was based on the 7th edition of the American Joint Committee on Cancer TNM classification. RCC grading was based on the Fuhrman nuclear grading system before 2014 and the International Society of Urological Pathology nucleolar grading system after 2014.
Patients initially received immunosuppressive therapy 2 days prior to KT. In patients with ABO incompatibility, a single dose of rituximab 200 mg was infused 14 to 21 days before KT, plasmapheresis was performed 4 to 9 times 7 to 14 days prior to KT until anti-A/B antibody titers decreased to below 1:8, and immunosuppressive drugs were initiated 7 to 10 days before KT. In HLA desensitization, the rituximab dose was 500 mg. The immunosuppressive drugs utilized were calcineurin inhibitors (tacrolimus or cyclosporine), corticosteroids (prednisolone or methyl-prednisolone), and antimetabolites (mycophenolate or azathioprine). Patients received induction therapy with anti-CD 25 monoclonal antibody (basiliximab, 20 mg) on the day of KT and postoperative day 4. The target trough level of tacrolimus was 8 to 10 ng/mL during the first year after KT and 5 to 8 ng/mL thereafter. The target cyclosporine trough level was 150 to 300 ng/mL during the first 3 months after KT and 100 to 150 ng/mL thereafter.
Data are presented as numbers and percentages or means ┬▒ standard deviations. The chi-square and FisherŌĆÖs exact tests were performed for categorical variables as appropriate, and the Mann-Whitney test was used for continuous variables. Patient survival and renal allograft survival were estimated by the Kaplan-Meier method with a log-rank test. All statistical tests were two-tailed, and a P value < 0.05 was considered statistically significant. Statistical analysis was performed using IBMŌĆōSPSS Statistics version 21.0 software (IBM Corp., Armonk, NY, USA).
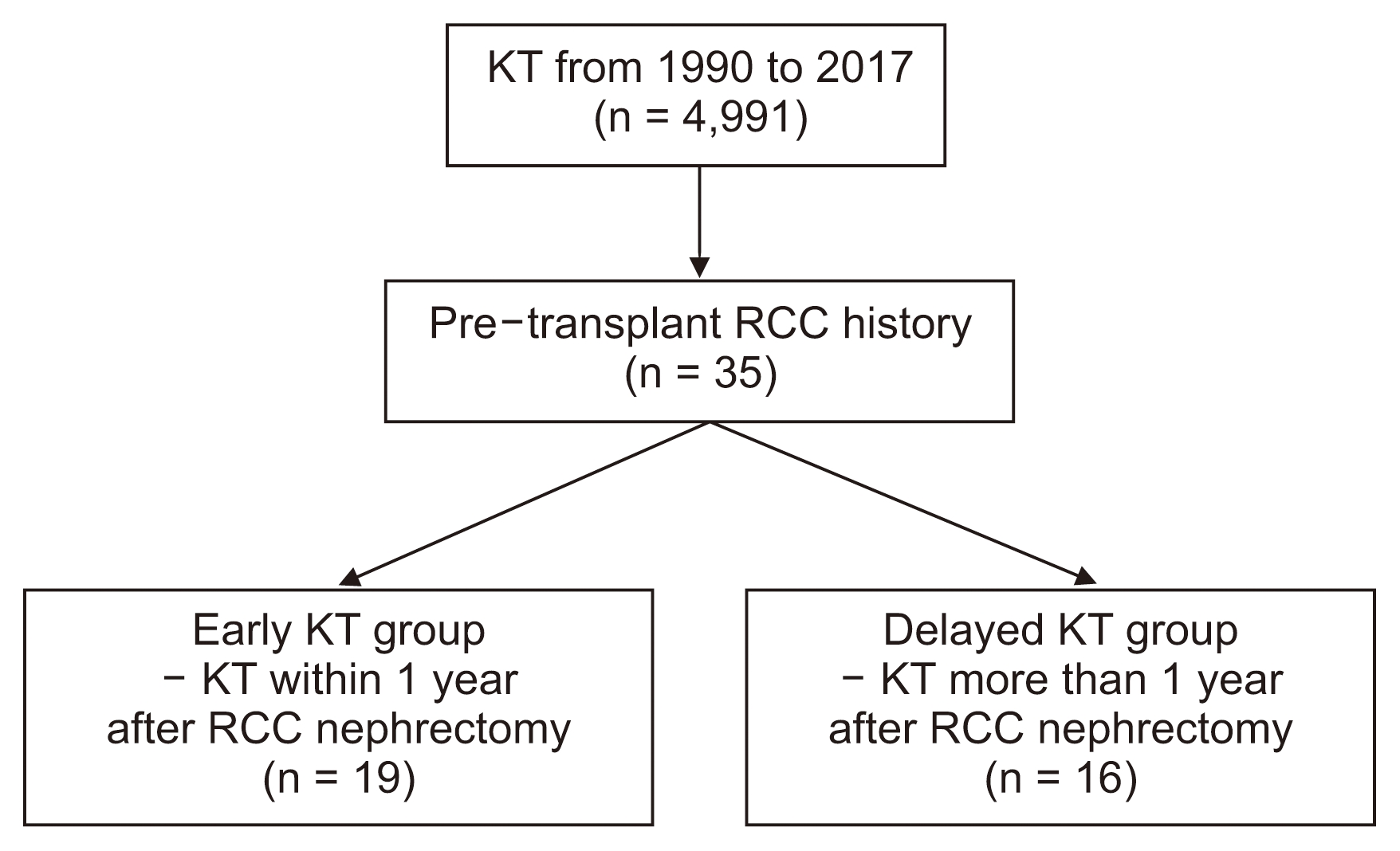
From 1990 to 2017, a total of 4,991 patients underwent KT at our center (Fig. 1). We identified 35 recipients aged 18 to 80 years who were diagnosed with RCC either prior to KT or after concomitant nephrectomy and KT. A total of 19 of the 35 recipients underwent KT within 1 year after nephrectomy, including 13 patients diagnosed with RCC by postoperative histopathologic examination after simultaneous KT and bilateral nephrectomy for cystic kidney diseases (CKDs; early KT group). The remaining 16 patients underwent KT > 1 year after nephrectomy (delayed KT group).
A total of 29 (82.9%) patients were male, and the mean age at RCC diagnosis was 45.71 ┬▒ 12.03 years (range, 18ŌĆō68; median, 45 years; Table 1). A total of 28 patients (80.0%) had renal failure due to nephropathy from diabetes (n = 5, 14.3%), hypertension (n = 6, 17.1%), glomerular diseases (n = 8, 22.9%), or polycystic kidney disease (PCKD, n = 9, 25.7%). Seven patients had bilateral RCC (20.0%) and were on chronic dialysis before the diagnosis of RCC and subsequent bilateral nephrectomy. Therefore, nephrectomy was not the cause of ESRD among either patients with an unspecified cause of CKD or those with bilateral RCC. The mean duration of dialysis before RCC diagnosis was 6.94 ┬▒ 4.78 months (range, 0ŌĆō15.70; median, 7.10 months). Baseline characteristics were not significantly different between the early and delayed KT groups.
A total of 22 (62.9%) patients underwent living-donor transplantation: 16 of 19 (84.2%) in the early KT group and 6 of 16 (37.5%) in the delayed KT group. The others underwent deceased donor transplantation. The difference in transplantation type between the early and delayed KT groups was statistically significant (P = 0.006). However, we did not find statistically significant differences in ABO incompatibility, HLA sensitization, HLA mismatch number, donor sex, or donor age.
A total of 24 patients (68.6%) used tacrolimus, and 11 (31.4%) used cyclosporine. A total of 31 (88.6%) patients received mycophenolate, and 6 (17.1%) received sirolimus after KT. There were no significant differences in the immunosuppressive drugs used between the early and delayed KT groups. The mean follow-up duration after KT was 50.71 ┬▒ 43.92 months (range, 3ŌĆō173; median, 38 months).
A total of 34 (97.1%) patients were diagnosed with T1N0M0 RCC, and 1 was diagnosed with T2N0M0. No patient had regional lymph node metastasis or distant metastasis. Clear cell carcinoma was the most common type of RCC (18/35, 51.4%), followed by acquired cystic disease (ACD)-associated RCC (10/35, 28.6%) and papillary cell RCC (6/35, 17.1%). Differences in tumor histology were statistically significant between the early and delayed KT groups (P = 0.036). ACD-associated RCC was the most common type (9/19, 47.4%) in the early KT group, whereas clear cell RCC was the most common type (10/16, 62.5%) in the delayed KT group (Table 2).
Bilateral RCCs were identified in 7 patients (20.0%), and 6 underwent KT within 1 year after bilateral nephrectomy; the remaining patient underwent KT 3 years after curative surgery. A total of 13 patients (37.1%) underwent simultaneous KT with bilateral or unilateral nephrectomy because of PCKD, ACD, or renal mass incidentally found at the time of transplant surgery; these RCCs were pathologically diagnosed postoperatively.
We did not find any confirmed RCC recurrence or de novo RCC in the remaining contralateral native kidney or transplant kidney during the postoperative follow-up. Patients in this study visited the urology department on a regular basis and underwent computed tomography (CT) or magnetic resonance imaging to monitor cancer recurrence for 5 years after nephrectomy for RCC. Even after 5 years of follow-up after nephrectomy, all patients, except one who was lost to follow-up, were monitored for RCC recurrence by CT or abdominal ultrasonography after KT. A total of 30 (85.7%) patients underwent follow-up; 4 (11.4%) were lost to follow-up, and 1 patient who underwent both KT and bilateral nephrectomy was diagnosed with unidentified metastatic adenocarcinoma determined unlikely to be RCC on bone biopsy. He died of metastatic cancer 6 months after KT.
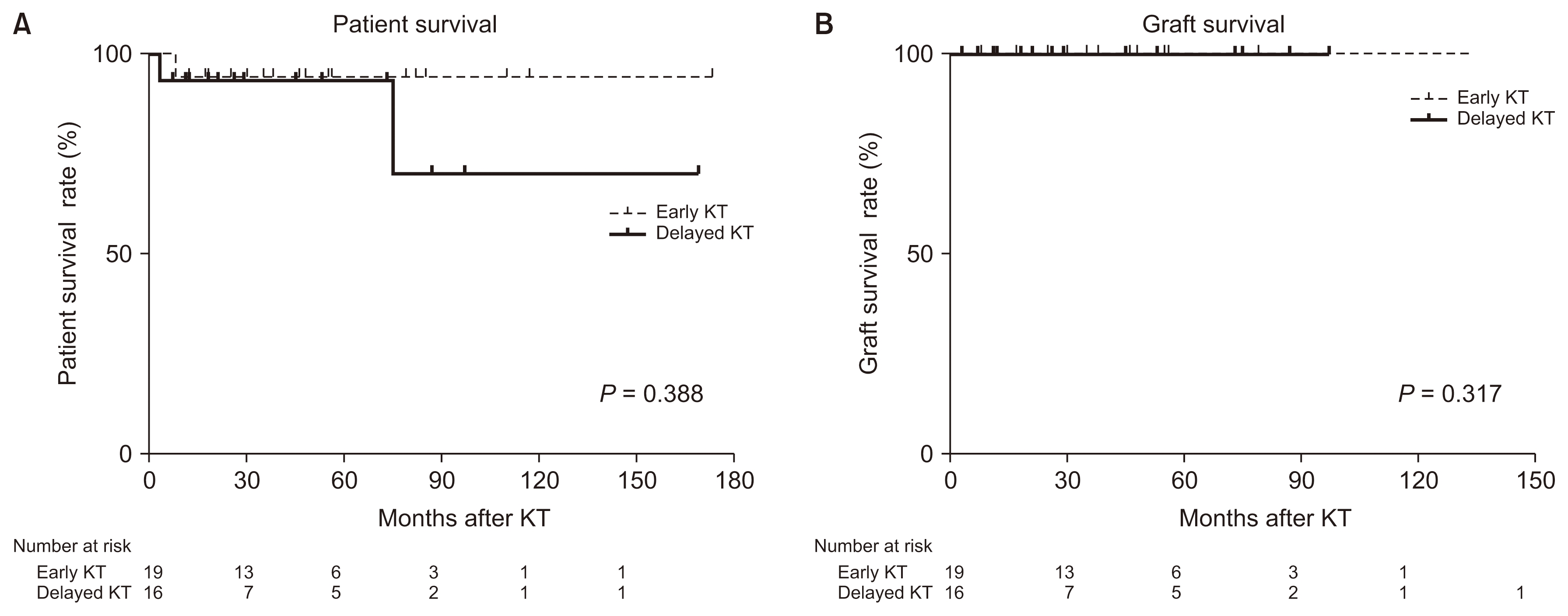
The overall 5- and 10-year patient survival rates were 94.1% and 84.7%, respectively. Three (8.6%) patients died during follow-up: two of septic shock and the other of metastatic cancer as mentioned above. The 10-year survival rates after KT were 94.7% in the early KT group and 70.3% in the delayed KT group. The difference in survival between the early and delayed KT groups was not statistically significant (P = 0.388) (Fig. 2A). Seven (20.0%) patients had biopsy-proven allograft rejection (Table 3). However, we identified only one graft failure (Fig. 2B).
KT has shown survival benefit and improved quality of life compared to dialysis in patients with ESRD [19,20]. However, cancer recurrence is a major concern in patients with ESRD and pretransplant malignancy, considering that they will receive immunosuppressive therapy [21,22]. Therefore, KT candidates are screened for malignant tumors, and RCC is detected occasionally. Previous studies have recommended a waiting time of 2 to 5 years for KT in patients with ESRD with RCC but suggested no delay in patients with asymptomatic and small RCC [12ŌĆō15]. However, this recommendation was based mainly on overseas studies. In Korea, there are insufficient data on transplant and cancer outcomes after KT in patients with RCC. Based on our clinical experience, we compared patient groups for 1 year to show that KT could be safely performed within 1 year after curative treatment for small and asymptomatic RCC without waiting for 2 to 5 years.
In this study, we evaluated patient survival, graft survival, rejection rate, and RCC recurrence in transplant recipients with RCC in a single center. Transplant and RCC outcomes were relatively positive. This is probably because of the fact that most patients had asymptomatic RCC diagnosed during the transplantation evaluation process or after a pathologic examination of specimens when nephrectomy was performed in conjunction with KT. Thirty-four patients had T1 RCC without lymphovascular invasion. Cognard et al [16] investigated RCC recurrence in 143 KT recipients with RCC; 9% had RCC recurrence and the 5- and 10-year incidence rates of recurrence after KT were 7.7% and 14.9%, respectively [16]. However, we did not observe any RCC recurrence in our study. The small sample size is one possible explanation. Low-stage cancer (97.1% of RCCs in our study were T1) and the fact that the patients were asymptomatic, except for two patients who presented with gross hematuria, are other possibilities. In a study by Cognard et al [16], early-stage RCCs showed better cancer outcome after transplantation.
We compared patient survival, allograft survival, and cancer recurrence between early and delayed KT; there were no significant differences. In a previous study on KT recipients with RCC, the overall survival was better in those with a shorter time to KT, but cancer-specific mortality was not affected by longer time [23]. In our study, 13 patients underwent KT in conjunction with nephrectomy (living donor, 10 patients; cadaveric donor, 3 patients); none were diagnosed with RCC before transplantation. After bilateral or unilateral nephrectomy due to PCKD, ACD, or incidental renal mass found at the time of transplant surgery, a pathologic examination revealed unilateral or bilateral RCC. These 13 patients did not have cancer recurrence after KT, and there was no difference in patient survival, graft survival, or graft rejection rate compared with patients who underwent KT > 1 year after nephrectomy for RCC. Therefore, a mandatory follow-up period for early-stage RCCs prior to KT is not clinically necessary, as has been previously published.
In our study, ACD-associated RCC was the most common type in the early KT group, whereas clear cell was the most common type in the delayed KT group. The early KT group had more frequent living donor KT than deceased donor KT. As RCC found in patients preparing for living donor KT developed in ESRD kidneys, we assumed that ACD-associated RCC was relatively more common than other types of RCC. In the delayed KT group, there were patients whose RCC was detected in CKD stages other than ESRD. Regarding baseline characteristics, living donor KT (84.2%) accounted for the majority of cases in the early KT group. This might be because most patients with asymptomatic and small RCC underwent nephrectomy at the time of transplant surgery in living donor KT.
The major limitation of this study is the relatively small sample size. However, to the best of our knowledge, this is the largest study in an Asian population to report the outcome of KT recipients with RCC. Our findings showed that KT can be safely performed with a short or no waiting time in patients with ESRD and RCC, and favorable outcomes can be obtained, especially in patients with early-stage cancer. The aforementioned French cohort study showed RCC recurrence after KT was associated with RCC stage, tumor pathology, and tumor grade [16]. As a result, we were unable to elicit a difference in cancer outcome and patient outcome according to the RCC stage and pathology. Clinicians may consider KT with nephrectomy in patients with ESRD and small asymptomatic or incidentally detected RCC.
Notes
AuthorsŌĆÖ contributions
Chung Hee Baek and Keun Hoi Park analyzed the data and drafted the manuscript. Jung A Yoon and Hak Soo Kim collected the data. Hyosang Kim, Su-Kil Park, Young Hoon Kim, Bumsik Hong, Dalsan You, and In Gab Jeong provided intellectual content of critical importance to the work. Chung Hee Baek designed and coordinated the study. All authors read and approved the final manuscript.
Figure┬Ā2
Outcomes in kidney transplant recipients with pre-transplant renal cell carcinoma. (A) Patient survival, (B) Graft survival.
KT, kidney transplantation.
Table┬Ā1
Baseline patient characteristics (n = 35)
Table┬Ā2
Histology and staging of renal cell carcinoma
References
1. Maisonneuve P, Agodoa L, Gellert R, et al. Cancer in patients on dialysis for end-stage renal disease: an international collaborative study. Lancet 1999;354:93ŌĆō99.


2. Stewart JH, Buccianti G, Agodoa L, et al. Cancers of the kidney and urinary tract in patients on dialysis for end-stage renal disease: analysis of data from the United States, Europe, and Australia and New Zealand. J Am Soc Nephrol 2003;14:197ŌĆō207.


3. Chow WH, Dong LM, Devesa SS. Epidemiology and risk factors for kidney cancer. Nat Rev Urol 2010;7:245ŌĆō257.



4. Ishikawa I, Saito Y, Shikura N, Kitada H, Shinoda A, Suzuki S. Ten-year prospective study on the development of renal cell carcinoma in dialysis patients. Am J Kidney Dis 1990;16:452ŌĆō458.


5. Breda A, Lucarelli G, Rodriguez-Faba O, et al. Clinical and pathological outcomes of renal cell carcinoma (RCC) in native kidneys of patients with end-stage renal disease: a long-term comparative retrospective study with RCC diagnosed in the general population. World J Urol 2015;33:1ŌĆō7.


6. Shrewsberry AB, Osunkoya AO, Jiang K, et al. Renal cell carcinoma in patients with end-stage renal disease has favorable overall prognosis. Clin Transplant 2014;28:211ŌĆō216.


7. Hashimoto Y, Takagi T, Kondo T, et al. Comparison of prognosis between patients with renal cell carcinoma on hemodialysis and those with renal cell carcinoma in the general population. Int J Clin Oncol 2015;20:1035ŌĆō1041.


8. Konnak JW, Grossman HB. Renal cell carcinoma as an incidental finding. J Urol 1985;134:1094ŌĆō1096.


9. Thompson IM, Peek M. Improvement in survival of patients with renal cell carcinoma--the role of the serendipitously detected tumor. J Urol 1988;140:487ŌĆō490.


10. Kessler O, Mukamel E, Hadar H, Gillon G, Konechezky M, Servadio C. Effect of improved diagnosis of renal cell carcinoma on the course of the disease. J Surg Oncol 1994;57:201ŌĆō204.


11. Ishikawa I, Honda R, Yamada Y, Kakuma T. Renal cell carcinoma detected by screening shows better patient survival than that detected following symptoms in dialysis patients. Ther Apher Dial 2004;8:468ŌĆō473.


12. Frasc├Ā GM, Brigante F, Volpe A, Cosmai L, Gallieni M, Porta C. Kidney transplantation in patients with previous renal cancer: a critical appraisal of current evidence and guidelines. J Nephrol 2019;32:57ŌĆō64.


13. Campbell S, Pilmore H, Gracey D, Mulley W, Russell C, Mc-Taggart S. KHA-CARI guideline: recipient assessment for transplantation. Nephrology (Carlton) 2013;18:455ŌĆō462.


14. Kasiske BL, Cangro CB, Hariharan S, et al. American Society of Transplantation. The evaluation of renal transplantation candidates: clinical practice guidelines. Am J Transplant 2001;1(Suppl 2):3ŌĆō95.

15. Knoll G, Cockfield S, Blydt-Hansen T, et al. Kidney Transplant Working Group of the Canadian Society of Transplantation. Canadian Society of Transplantation consensus guidelines on eligibility for kidney transplantation. CMAJ 2005;173:1181ŌĆō1184.



16. Cognard N, Anglicheau D, Gatault P, et al. Recurrence of renal cell cancer after renal transplantation in a multicenter French cohort. Transplantation 2018;102:860ŌĆō867.


17. Znaor A, Lortet-Tieulent J, Laversanne M, Jemal A, Bray F. International variations and trends in renal cell carcinoma incidence and mortality. Eur Urol 2015;67:519ŌĆō530.


18. Olshan AF, Kuo TM, Meyer AM, Nielsen ME, Purdue MP, Rathmell WK. Racial difference in histologic subtype of renal cell carcinoma. Cancer Med 2013;2:744ŌĆō749.



19. Wolfe RA, Ashby VB, Milford EL, et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 1999;341:1725ŌĆō1730.


20. Liem YS, Weimar W. Early living-donor kidney transplantation: a review of the associated survival benefit. Transplantation 2009;87:317ŌĆō318.


21. Penn I. The effect of immunosuppression on pre-existing cancers. Transplantation 1993;55:742ŌĆō747.





 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print
















