| Kidney Res Clin Pract > Volume 38(3); 2019 > Article |
|
Abstract
Central venous disease (CVD) is difficult to treat and often resistant to treatment. In CVD, hemodialysis vascular access should sometimes be abandoned, or in serious cases, the patient's life may be threatened. Therefore, prevention is ideal. However, as the prevalence of chronic kidney disease (CKD) has increased steadily with population aging, CKD patients with a peripherally inserted central catheter (PICC) are encountered frequently. PICCs can cause CVD, and the basilic vein, which is regarded as the important last option for native arteriovenous fistula (AVF) creation in end-stage renal disease (ESRD) patients, is destroyed frequently after its use as the entry site of PICC. The most well-established risk factors for CVD are a history of central venous catheter (CVC) insertion and its duration of use. Therefore, to reduce the incidence of CVD, catheterization in the central vein (CV) should be minimized, along with its duration of use. In this review, we will first explain the basic territories of the CV and introduce its pathophysiology, clinical features, and advanced treatment options. Finally, we will emphasize prevention of CVD.
Central venous disease (CVD) represents a pathological condition in which stenosis or occlusion occurs in the central vein (CV) [1]. The well-known cause of CVD is the presence of history of central venous catheter (CVC) insertion. As the use of peripherally inserted central catheter (PICC) has been rapidly increasing recently, more attention should be paid to CVD. Although superior vena cava (SVC) syndrome can be caused by a tumor invading the mediastinum, there is often no symptom in non-hemodialysis (HD) patients with CVD and limited venous blood flow volume [2]. However, in end-stage renal disease (ESRD) patients with HD, because a large blood flow volume of vascular access (VA) eventually passes through the CV, CVD often manifests as edema. Studies on treatment of symptomatic CVD have been most common in HD patients [3,4]. CVD patients may not be good candidates for surgery due to lesion presence in the thorax, and such patients are more likely to have multiple co-morbidities [5]. Endovascular intervention, especially the use of stent-grafts (SG), seems promising, but prevention of CVD is most important.
In clinical practice, as the prevalence of chronic kidney disease (CKD) has been increasing steadily as the population ages, CKD patients from other departments who are using PICC are encountered frequently [6]. PICC can cause CVD, and the basilic vein, which is the important last option for native arteriovenous fistula (AVF) creation in ESRD patients, is destroyed frequently after its use as the entry site of PICC [7]. Therefore, the purpose of this review is to introduce guidelines to prevent CVD for non-nephrology physicians. All materials for radiologic and photographic figures in this article were approved by the Institutional Review Board (IRB) of St. Vincent’s Hospital, The Catholic University of Korea (IRB No. VC19RESE0062). Facial exposures were very limited to guarantee anonymity.
The central venous system comprises the superior and inferior vena cava and right and left brachiocephalic, subclavian, internal jugular, and iliac veins. However, it does not include axillary, femoral, or external jugular veins (Fig. 1). CVD can be divided into cases associated with previous catheter insertion and those not associated with previous catheter insertion [8,9].
Cases associated with previous catheter insertion often experience stenosis or occlusion. The most well-known risk factor associated with CVD is duration of catheter insertion. The longer is the period of insertion in the vein, the greater is the probability of central venous stenosis or occlusion. There are reports that number of catheter insertions and size of the catheter are also related, but no firm conclusions have been established [10].
In cases not associated with previous catheter insertion, turbulent VA blood flow damages the vessel wall and causes stenosis of the CV. Left brachiocephalic vein (BCV) stenosis is a good example of this phenomenon. In left BCV, stenosis usually occurs at two points, the junction of the left subclavian vein (SCV) and internal jugular vein (IJV) and the junction of the left BCV with the right BCV extending to the SVC. Furthermore, the left BCV is located between the sternum and pulsating aorta, which also contributes to stenosis. For similar anatomical reasons, a catheter inserted into the left IJV, in contrast to the right IJV, should be bent and will often contact the vessel wall at the two places mentioned above along its path to the right atrium (RA) (Fig. 2). Such catheter contact damages the vessel wall and causes stenosis.
Also, because the SCV is located between the clavicle and the first rib, catheter insertion into the SCV causes frequent stenosis, which is why the IJV is used as the entry site for long-term HD catheter insertion.
Clinical features may vary according to lesion location, but the closer the lesion is to the RA, the more severe is the clinical feature. The most common clinical manifestation of CVD in HD patients is arm edema (Fig. 3).
Although SCV catheterization for HD is prohibited, SCV stenosis can occur after diagnostic angiography due to edema of the arm. In such cases, stenoses are often observed at the junction of the SCV and the IJV, resulting in turbulent venous blood flow. In some cases, this is diagnosed as a form of thoracic outlet syndrome (TOS) when the SCV is compressed between the clavicle and the first rib.
Stenosis or occlusion of one BCV manifests as ipsilateral arm and facial edema (Fig. 4, 5), but swelling of the face or arm may not be obvious if collateral veins are abundant.
The presence of collateral veins is an important factor affecting awareness of the clinical manifestations of CVD (Fig. 6). These collateral veins include intercostal, azygos, hemiazygos, and accessory hemiazygos veins. In cases of abundant collateral flow to the intercostal veins, ipsilateral breast swelling can be the manifestation of CVD.
Problems related to HD VA affect the survival rate of ESRD patients. Various techniques of endovascular therapy resulted in a breakthrough development in the treatment of HD VA [11–13]. However, the lesion of CV is much less responsive to endovascular therapy than that of a peripheral location. Nevertheless, endovascular therapy is preferred in CVD because of the surgical limitation due to lesion presence in the thorax, and ESRD patients are older and frequently have multiple comorbidities [14].
Percutaneous transluminal angioplasty (PTA) with balloon dilatation is the primary basis for endovascular therapy. However, balloon dilation should be performed only if there is a clinical indication such as arm or face swelling. Several studies have reported that balloon dilation for a narrowed lesion found incidentally on angiogram and without symptoms accelerates lesion growth [15–17].
If symptoms are present, PTA is performed; however, patency is poor, so repeat procedures are often required. Therefore, in many cases, the stent or SG is inserted later [18]. Because the diameter of the CV is larger than that of the peripheral vein, balloon dilatation may not efficiently dilate and correct the lesion. Recent studies using intravascular ultrasound (IVUS) for CVD showed that, although the lesion was sufficiently enlarged on angiography after PTA, IVUS demonstrated insufficient dilation or extrusion by the balloon catheter [19]. In such cases, additional PTA using a larger balloon catheter can be considered, but the risk of vessel rupture may also increase, requiring attention to the possibility of CV rupture. Although stent use in the venous system is expected to have a good result, as in cases of coronary or peripheral arteries, numerous studies showed failure of stent use, especially in HD VA, because of neointimal hyperplasia (NIH) within the stent, leading to a lower patency rate than that of PTA [20,21]. However, stent or SG use in complete CV occlusion can be considered as a guiding role for subsequent procedures if recanalization is achieved. The SG is a structure that applies graft material to the inside or outside of the stent to create a physical barrier to NIH. SG use seems promising in CVD because it has been consistently reported to have a better patency rate than stent alone or PTA [20,22–24]. In particular, in CVD, SG use showed favorable patency compared with PTA in several retrospective studies, although no prospective studies have been published yet. Table 1 shows a summary of the studies on SG use in HD CVD [3,18,22,25,26].
However, SG use has limitations in that edge stenosis can develop at either end, increasing medical costs. Because the SG is inserted where two veins meet, one vein can be blocked, and the corresponding vein cannot be used to create a new AVF; thus, attention should be paid when inserting a SG in such a location (Fig. 7).
As in coronary and peripheral artery diseases, the use of drug-coated balloon (DCB) in HD VA has been studied extensively and showed some benefits. However, most of those studies excluded CVD because of the absence of a large-diameter DCB. There are only two studies of DCB use in CVD [27,28], each of which demonstrated benefits. However, in the meta-analysis of these two studies, the benefit was no longer observed. Based on personal experiences in CVD intervention, an elastic recoil phenomenon is frequently noted, and it has been suggested that insufficient luminal gain is achieved by PTA based on IVUS [19,29]. Therefore, the benefit of DCB in CVD seems limited.
Surgical options for CVD can be divided into three categories: inflow reduction, unusual bypass including reconstruction surgery and claviculectomy, or first rib resection in TOS [30].
There are some studies about inflow reduction including HD patients with high output cardiac status, but only one study focused on inflow reduction in HD patients with CVD [31]. Inflow can be reduced by non-surgical banding or various surgical techniques including plication, graft banding or wrapping, and graft interposition. Development of CVD can be explained by inflow-outflow mismatch, indicating the importance of inflow reduction. However, to maximize its efficacy, inflow volume should be sufficiently reduced. For this, intraoperative volume measurement using duplex ultrasound should be performed during volume reduction [32,33].
Unusual bypass surgeries include simple bypass using a graft to the ipsilateral jugular vein or bypass to the contralateral jugular, axillary, or femoral vein in a lower extremity. Furthermore, direct connection to the SVC or RA can be performed, but such surgeries are not simple and confer risk and complications. Sophisticated surgical options can be actively considered in non-elderly patients without comorbidities or when SG is unavailable. However, in clinical practice, HD patients are getting older and frequently have multiple comorbidities such that risk vs. benefits for surgical options should be discussed with the patient and a vascular surgeon. A multidisciplinary approach is important and required, especially in CVD.
Closure of a corresponding HD VA is the simplest and most reliable surgical option. However, it is not easy to determine this, because HD VA is a lifeline in these patients, and there are limited available veins in the human body (Fig. 8).
During surgery for CVD, VA sometimes should be abandoned to avoid life-threatening complications. Therefore, the most effective method is CVD prevention. Although the Kidney Disease Outcomes Quality Initiative (KDOQI) guidelines suggest venous preservation for native AVF creation to begin at CKD stage 4 [34], the American Society of Diagnostic and Interventional Nephrology (ASDIN) and Association of Vascular Access (AVA) recommend that venous preservation start at CKD stage 3 [35]. For similar reasons, use of PICC is prohibited starting in CKD stage 3. CKD stage is classified according to estimated glomerular filtration rate (eGFR), which is automatically calculated through a formula such as the Modification of Diet in Renal Disease (MDRD) equation using parameters including serum creatinine, age, sex, and race. However, because serum creatinine level is more familiar to non-nephrology physicians than eGFR, serum creatinine 2.0 mg/dL or higher is recommended as a standard for venous preservation, and PICC use should be prohibited non-nephrology physicians. For subclavian catheterization, the same rule can be applied. Although it is well recognized among nephrologists that subclavian catheterization should not be performed in CKD patients, it still occurs frequently. Therefore, non-nephrology physicians should be instructed to avoid this procedure.
Various treatment options are currently being tried for CVD, but all have limitations. Therefore, prevention is ideal. First, catheterization should be minimized in CV, as its performance is a well-known cause of CVD. It is also important to minimize the duration of CVC use. Finally, use of the right IJV with a straight path should always be considered rather than the left IJV with curvature. In addition, treatment of CV lesions may accelerate its progression, and treatment must be performed with care.
Figure 1
Anatomy of the venous system showing central veins in addition to the veins of the proximal part of upper and lower extremities.

Figure 2
Right-side inserted catheter into the right internal jugular vein (IJV) with a straight path (A) and left-side inserted catheter into left IJV with multiple curves (B).
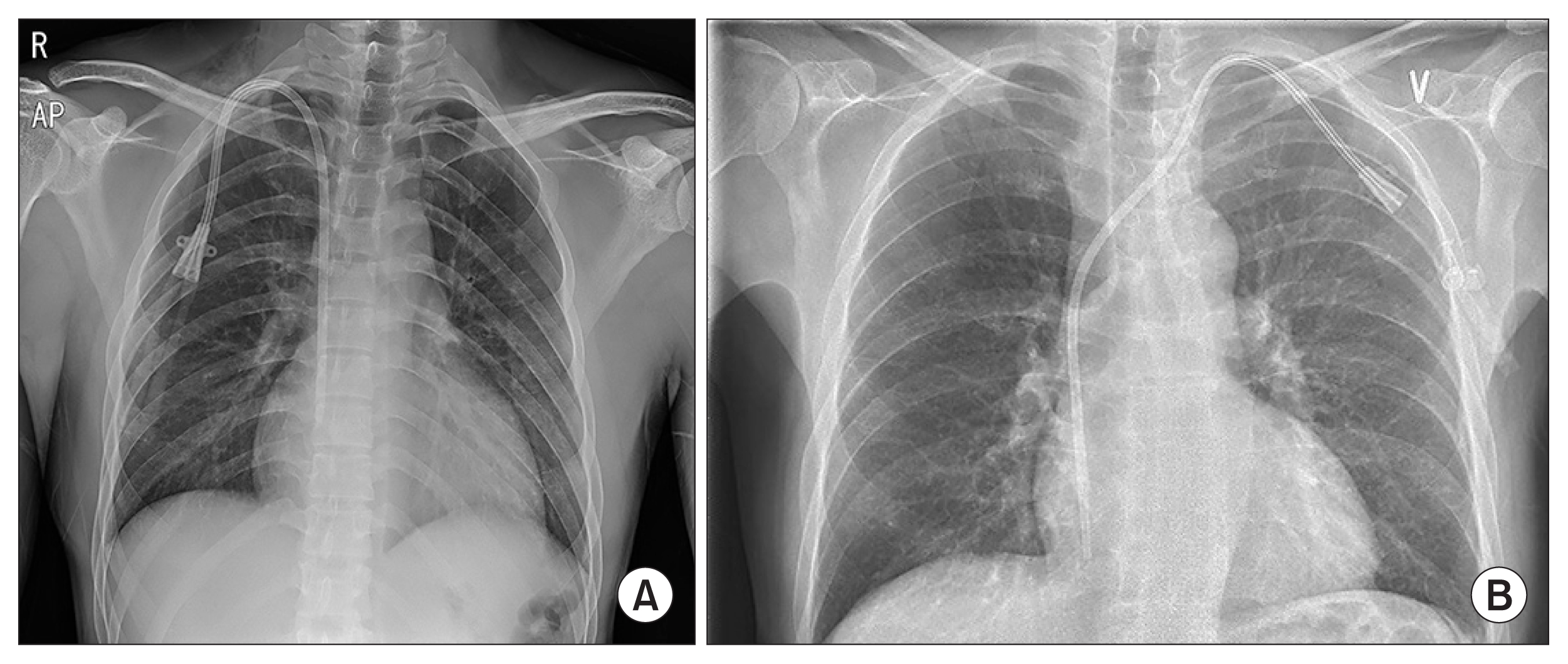
Figure 3
Left brachiocephalic vein (BCV) stenosis.
Left BCV stenosis documented in angiography caused ipsilateral arm swelling compared with the normal-sized right arm in a hemodialysis patient.
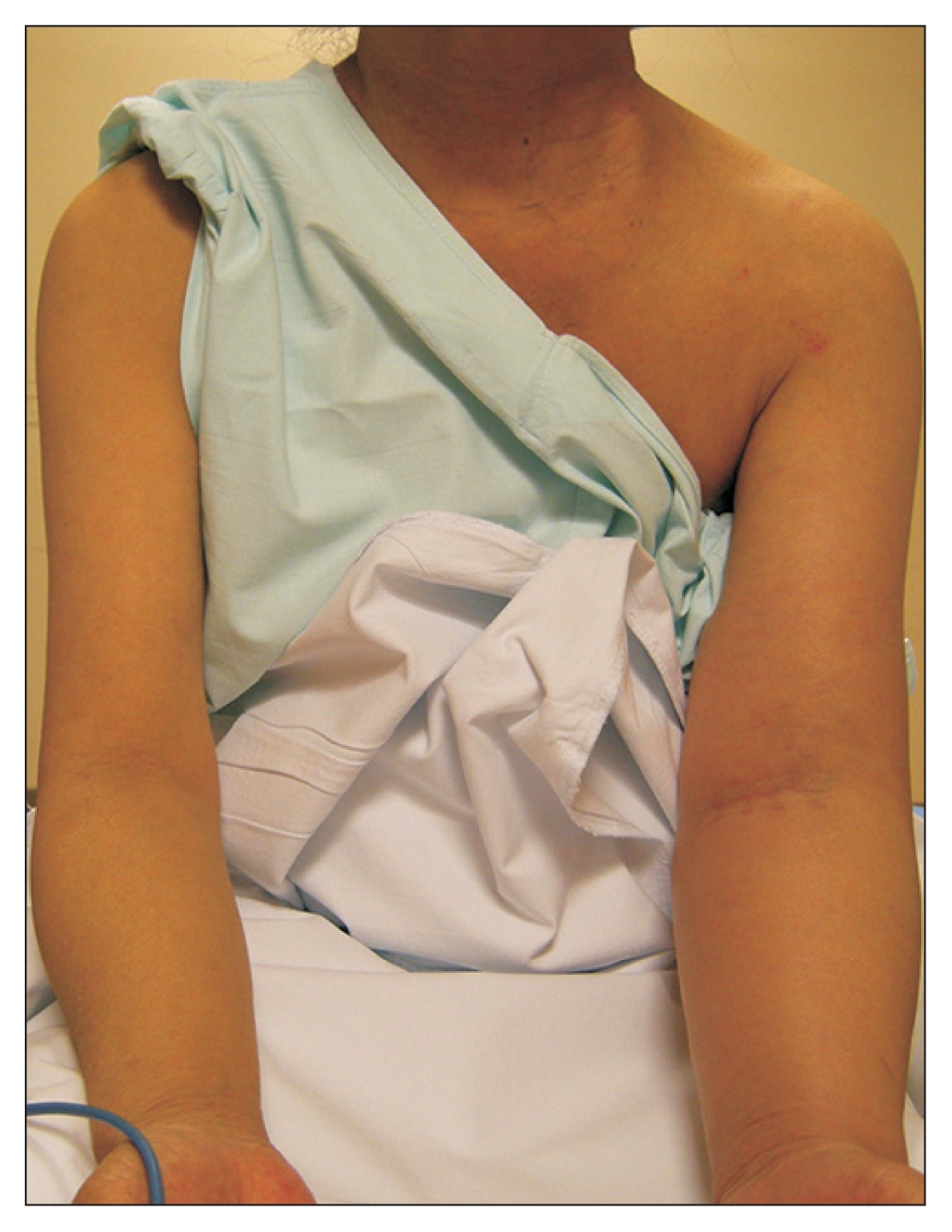
Figure 4
Right brachiocephalic vein (BCV) stenosis.
Facial swelling (A) manifested in this patient, which was caused by hemodialysis (HD) catheter insertion into the stenosed right BCV documented in angiography (B). It resolved with HD catheter removal (C) and subsequent percutaneous transluminal angioplasty on right BCV after arteriovenous fistula maturation (D).
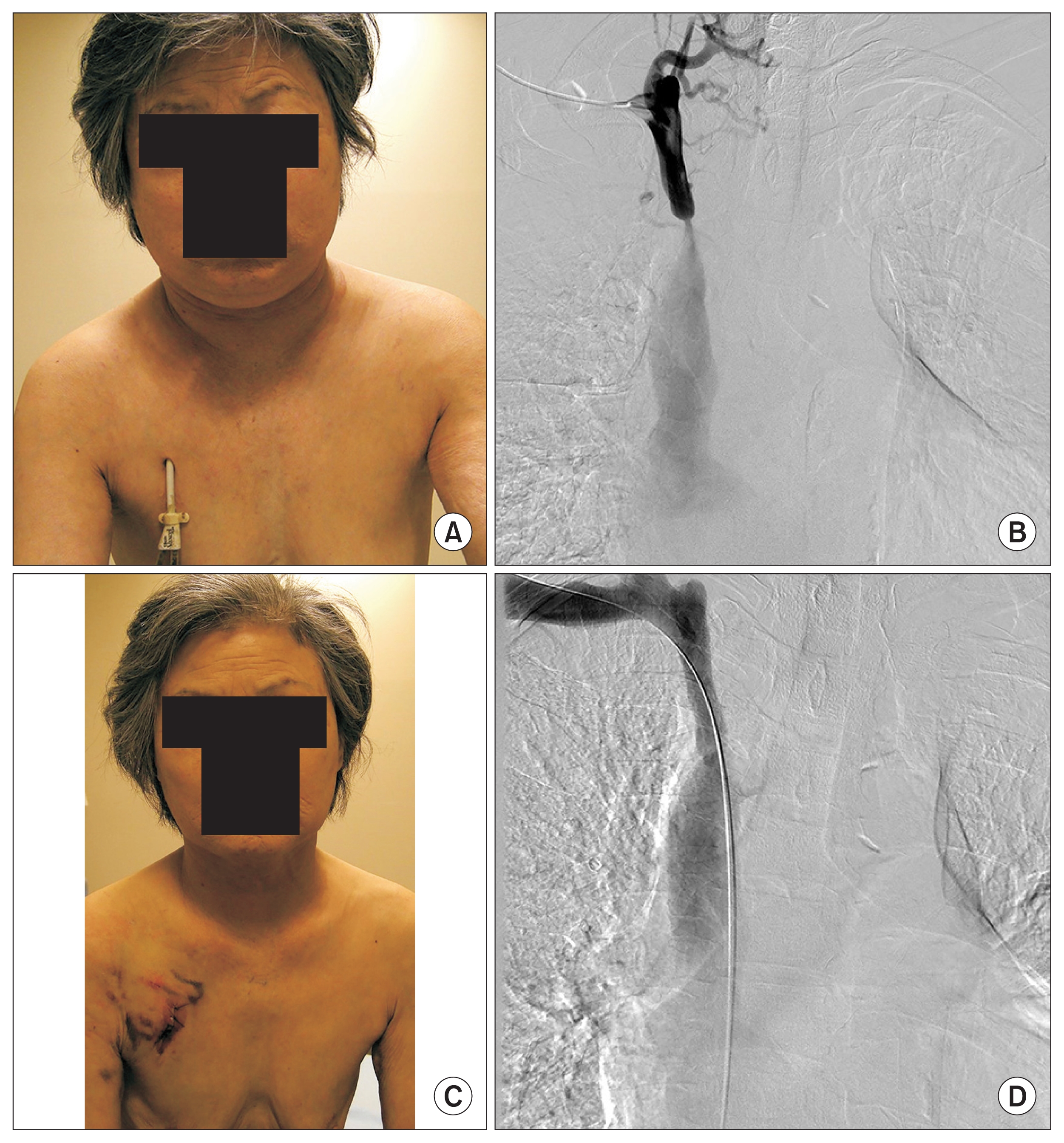
Figure 5
Superior vena cava (SVC) syndrome.
Facial swelling manifested (A) after left-side inserted hemodialysis (HD) catheter insertion into the stenosed SVC, confirmed in chest computed tomography (B). It resolved with HD catheter removal (C).
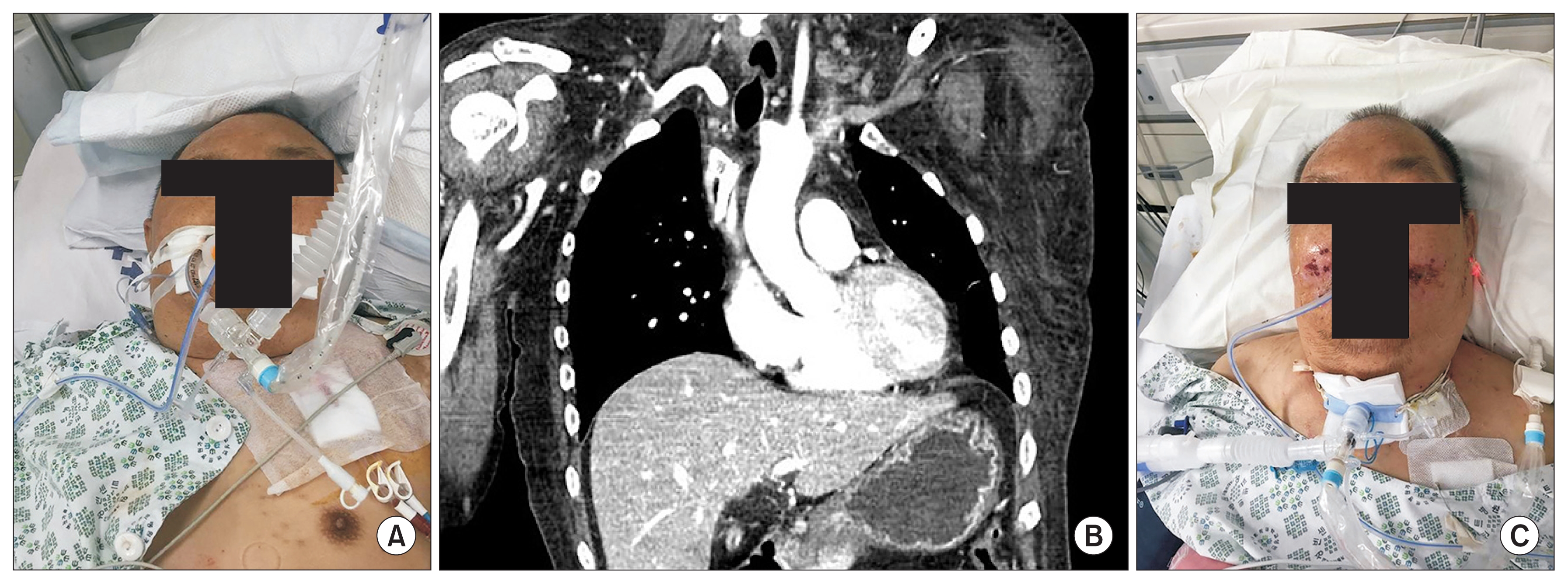
Figure 6
Asymptomatic central vein disease.
Multiple collateral veins with diffuse stenosis in the right subclavian vein and complete occlusion in the right brachiocephalic vein visualized in angiography in a hemodialysis patient with no complaint about arm swelling.

Figure 7
Jailing vs. without jailing.
Right internal jugular vein (IJV) was jailed by Bare metal stent (a 10-mm-diameter×100-mm-long Wall-stent Endoprosthesis; Boston Scientific, Marlborough, MA, USA) placement in the right subclavian vein so that it cannot be accessible for the further catheter insertion (A). Stent-graft (a 12-mm-diameter×60-mm-long Hercules Vascular; S&G Biotech, Yongin, Korea) was successfully deployed on the left brachiocephalic vein (BCV) stenosis without jailing of the right BCV in a symptomatic hemodialysis patient with left arm swelling (B).
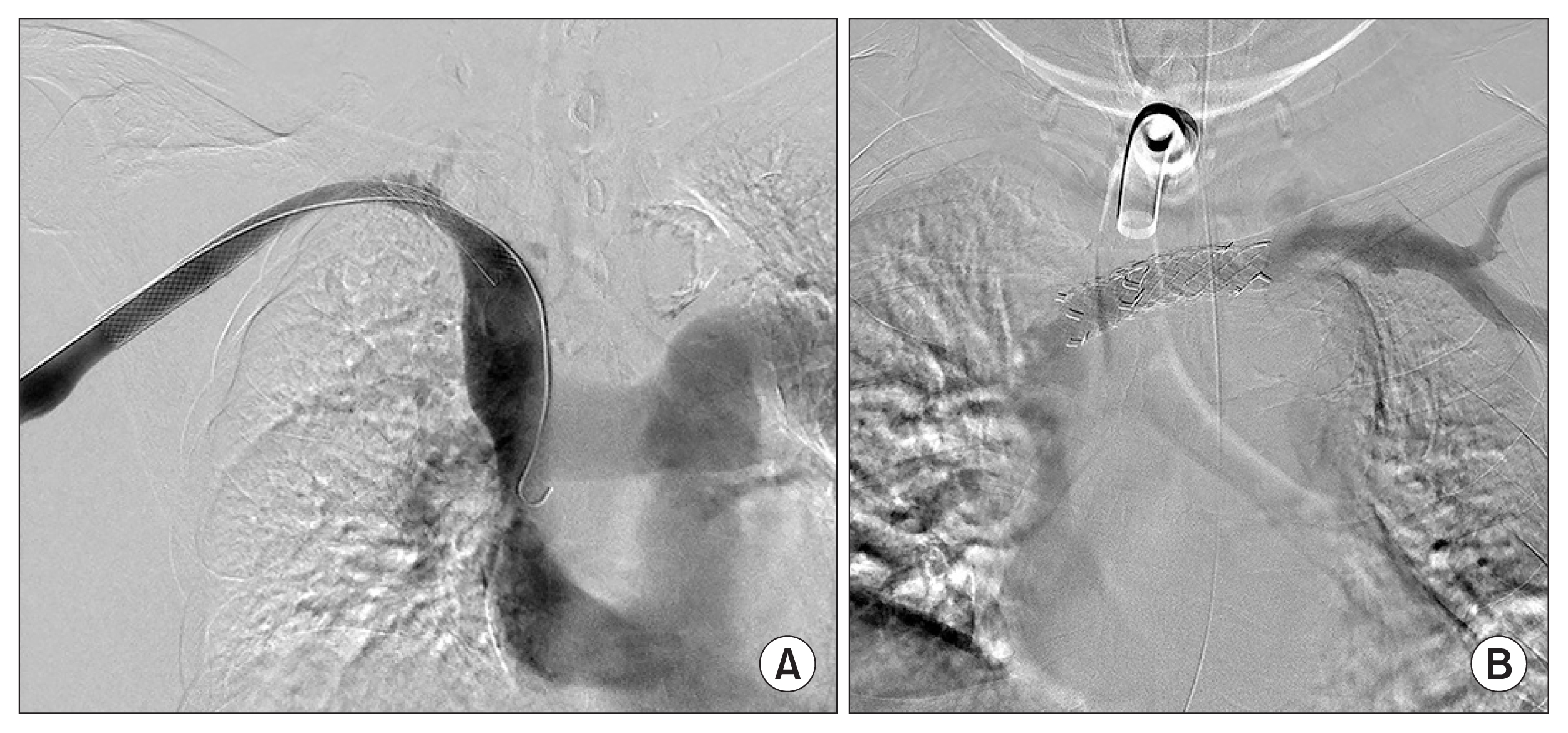
Figure 8
Treatment flow diagram in CVD.
AVF, arteriovenous fistula; BMS, bare metal stent; CVD, central vein disease; PTA, percutaneous transluminal angioplasty; Qac, vascular access flow volume; TOS, thoracic outlet syndrome; VA, vascular access.
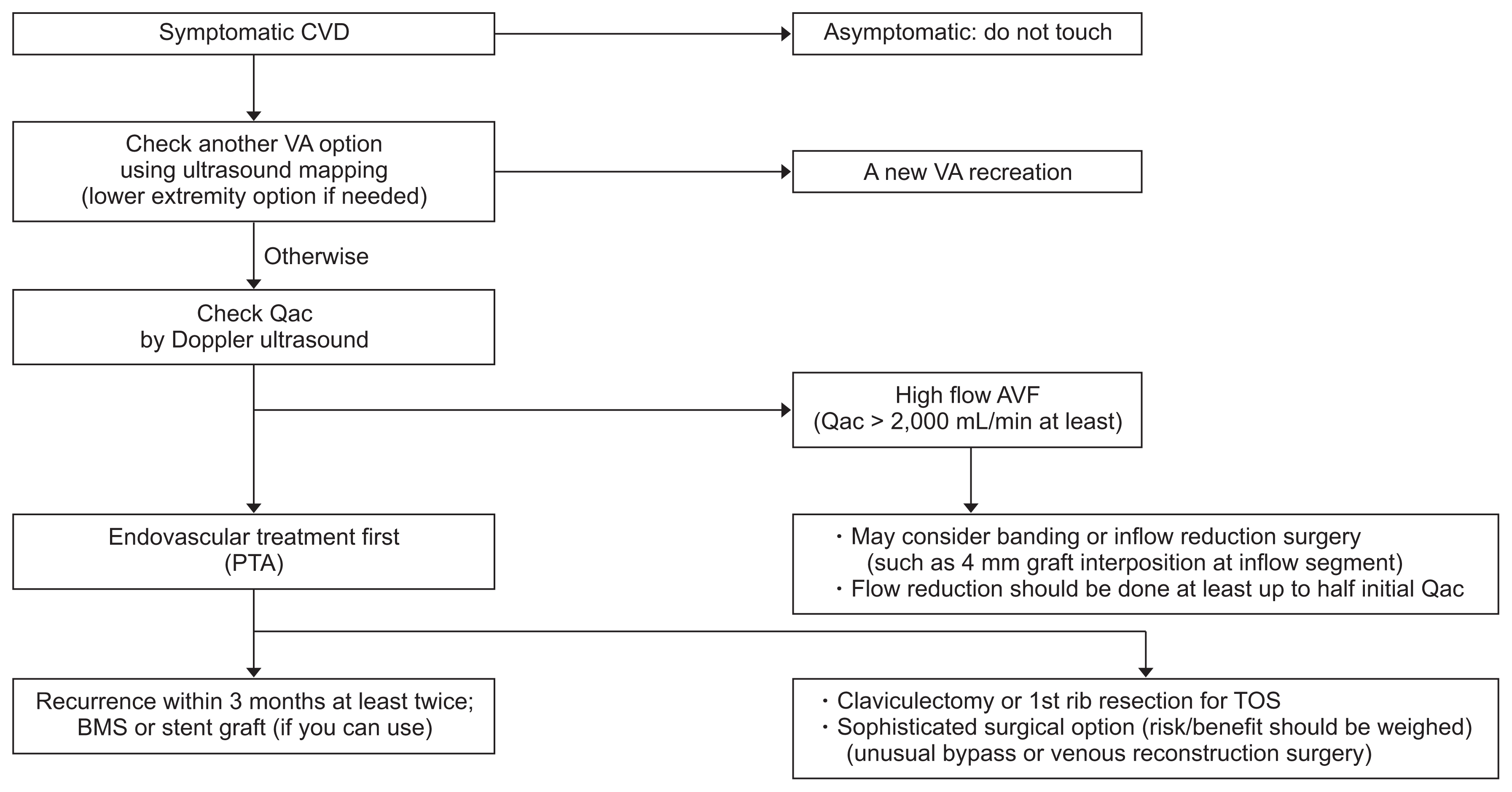
Table 1
Summary of primary and primary assisted patencies of SG in HD VA studies
| Study | Type of SG | Number of patients | Primary/primary assisted patencies (%) | ||
|---|---|---|---|---|---|
|
|
|||||
| 6 mo | 12 mo | 24 mo | |||
| Kundu et al [25] | Fluency | 14 | 100/NA | NAa/NA | NA/NA |
| Anaya-Ayala et al [22] | Viabahnb | 25 | NA/NA | 56/86 | NA/NA |
| Jones et al [3] | Viabahn | 30 | 81/100 | 67/80 | 45/75 |
| Verstandig et al [26] | Viabahn & Fluencyb | 52 | 60/96 | 40/94 | 28/85 |
| Quaretti et al [18] | Variousc | 20 | 100/NA | 100/NA | 84/NA |
References
2. Agarwal AK, Khabiri H, Haddad NJ. Complications of vascular access: superior vena cava syndrome. Am J Kidney Dis 2017;69:309–313.


3. Jones RG, Willis AP, Jones C, McCafferty IJ, Riley PL. Long-term results of stent-graft placement to treat central venous stenosis and occlusion in hemodialysis patients with arteriovenous fistulas. J Vasc Interv Radiol 2011;22:1240–1245.


4. Falk A, Maya ID, Yevzlin AS. RESCUE Investigators. A prospective, randomized study of an expanded polytetrafluoroethylene stent graft versus balloon angioplasty for instent restenosis in arteriovenous grafts and fistulae: two-year results of the RESCUE study. J Vasc Interv Radiol 2016;27:1465–1476.


5. Jin DC, Yun SR, Lee SW, Han SW, Kim W, Park J. Current characteristics of dialysis therapy in Korea: 2015 registry data focusing on elderly patients. Kidney Res Clin Pract 2016;35:204–211.



6. El Ters M, Schears GJ, Taler SJ, et al. Association between prior peripherally inserted central catheters and lack of functioning arteriovenous fistulas: a case-control study in hemodialysis patients. Am J Kidney Dis 2012;60:601–608.



7. McGill RL, Ruthazer R, Meyer KB, Miskulin DC, Weiner DE. Peripherally inserted central catheters and hemodialysis outcomes. Clin J Am Soc Nephrol 2016;11:1434–1440.



8. Agarwal AK, Patel BM, Haddad NJ. Central vein stenosis: a nephrologist’s perspective. Semin Dial 2007;20:53–62.


9. Kundu S. Central venous disease in hemodialysis patients: prevalence, etiology and treatment. J Vasc Access 2010;11:1–7.

10. Chick JF, Reddy SN, Yam BL, Kobrin S, Trerotola SO. Institution of a hospital-based central venous access policy for peripheral vein preservation in patients with chronic kidney disease: a 12-year experience. J Vasc Interv Radiol 2017;28:392–397.


11. Park HS, Lee YH, Kim HW, et al. Usefulness of assisted procedures for arteriovenous fistula maturation without compromising access patency. Hemodial Int 2017;21:335–342.


12. Cho S. The feasibility of surgical salvage of thrombosed arteriovenous fistula by an interventional nephrologist. Kidney Res Clin Pract 2017;36:175–181.



13. Cho S, Lee YJ, Kim SR. Clinical experience with ultrasound guided angioplasty for vascular access. Kidney Res Clin Pract 2017;36:79–85.



14. Jin DC, Yun SR, Lee SW, et al. Current characteristics of dialysis therapy in Korea: 2016 registry data focusing on diabetic patients. Kidney Res Clin Pract 2018;37:20–29.



15. Levit RD, Cohen RM, Kwak A, et al. Asymptomatic central venous stenosis in hemodialysis patients. Radiology 2006;238:1051–1056.


16. Ehrie JM, Sammarco TE, Chittams JL, Trerotola SO. Unmasking of previously asymptomatic central venous stenosis following percutaneous transluminal angioplasty of hemodialysis access. J Vasc Interv Radiol 2017;28:1409–1414.


17. Yan Y, Sudheendra D, Dagli MS, et al. Effect of central venous angioplasty on hemodialysis access circuit flow: prospective study of 25 symptomatic patients. J Vasc Interv Radiol 2015;26:984–991.


18. Quaretti P, Galli F, Moramarco LP, et al. Stent grafts provided superior primary patency for central venous stenosis treatment in comparison with angioplasty and bare metal stent: a retrospective single center study on 70 hemodialysis patients. Vasc Endovascular Surg 2016;50:221–230.


19. de Graaf R, van Laanen J, Peppelenbosch N, van Loon M, Tordoir J. The value of intravascular ultrasound in the treatment of central venous obstructions in hemodialysis patients. J Vasc Access 2016;17(Suppl 1):S12–S15.


20. Haskal ZJ, Trerotola S, Dolmatch B, et al. Stent graft versus balloon angioplasty for failing dialysis-access grafts. N Engl J Med 2010;362:494–503.


21. Salman L, Asif A. Stent graft for nephrologists: concerns and consensus. Clin J Am Soc Nephrol 2010;5:1347–1352.


22. Anaya-Ayala JE, Smolock CJ, Colvard BD, et al. Efficacy of covered stent placement for central venous occlusive disease in hemodialysis patients. J Vasc Surg 2011;54:754–759.


23. McLennan G. Stent and stent-graft use in arteriovenous dialysis access. Semin Intervent Radiol 2016;33:10–14.



24. Patel D, Ray CE Jr, Lokken RP, Bui JT, Lipnik AJ, Gaba RC. Advanced stent graft treatment of venous stenosis affecting hemodialysis vascular access: case illustrations. Semin Intervent Radiol 2016;33:39–45.



25. Kundu S, Modabber M, You JM, Tam P, Nagai G, Ting R. Use of PTFE stent grafts for hemodialysis-related central venous occlusions: intermediate-term results. Cardiovasc Intervent Radiol 2011;34:949–957.


26. Verstandig AG, Berelowitz D, Zaghal I, et al. Stent grafts for central venous occlusive disease in patients with ipsilateral hemodialysis access. J Vasc Interv Radiol 2013;24:1280–1287.


27. Kitrou PM, Papadimatos P, Spiliopoulos S, et al. Paclitaxel-coated balloons for the treatment of symptomatic central venous stenosis in dialysis access: results from a randomized controlled trial. J Vasc Interv Radiol 2017;28:811–817.


28. Massmann A, Fries P, Obst-Gleditsch K, Minko P, Shayesteh-Kheslat R, Buecker A. Paclitaxel-coated balloon angioplasty for symptomatic central vein restenosis in patients with hemodialysis fistulas. J Endovasc Ther 2015;22:74–79.


29. Ross JR, Franga DL, Gallichio M, Patel AJ, Ouriel K. Role of intravascular ultrasound imaging during endovascular interventions of failing hemodialysis access grafts. J Vasc Surg 2017;65:1383–1389.


30. Anaya-Ayala JE, Bellows PH, Ismail N, et al. Surgical management of hemodialysis-related central venous occlusive disease: a treatment algorithm. Ann Vasc Surg 2011;25:108–119.


31. Jennings WC, Miller GA, Coburn MZ, Howard CA, Lawless MA. Vascular access flow reduction for arteriovenous fistula salvage in symptomatic patients with central venous occlusion. J Vasc Access 2012;13:157–162.


32. Zanow J, Petzold K, Petzold M, Krueger U, Scholz H. Flow reduction in high-flow arteriovenous access using intraoperative flow monitoring. J Vasc Surg 2006;44:1273–1278.


33. Tellioglu G, Berber I, Kilicoglu G, Seymen P, Kara M, Titiz I. Doppler ultrasonography-guided surgery for high-flow hemodialysis vascular access: preliminary results. Transplant Proc 2008;40:87–89.


34. Vascular Access 2006 Work Group. Clinical Practice Guidelines for Vascular Access. Am J Kidney Dis 2006;48(Suppl 1):S176–S247.


35. Hoggard J, Saad T, Schon D, Vesely TM, Royer T. American Society of Diagnostic and Interventional Nephrology, Clinical Practice Committee; Association for Vascular Access. Guidelines for venous access in patients with chronic kidney disease. A Position Statement from the American Society of Diagnostic and Interventional Nephrology, Clinical Practice Committee and the Association for Vascular Access. Semin Dial 2008;21:186–191.

- TOOLS
-
METRICS

- Related articles
-
Target blood pressure in Korean hemodialysis patients for optimal survival
Clinical influencing factors affecting pulmonary hypertension in hemodialysis patients
COVID-19–related clinical outcomes among Korean hemodialysis patients2022 September;41(5)
Humoral response to viral vector COVID-19 vaccine in hemodialysis patients2022 May;41(3)
Sexual Functioning in Male Hemodialysis Patients2011 January;30(1)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print















